Natural Sleep Solutions
March 5, 2012 Written by JP [Font too small?]According to a recent review in the journal The Lancet, disturbed sleep and insomnia affect upwards of 25% of the adult population. Not only does this impact quality of life, but it also predisposes those with sleep disorders to a much higher risk of numerous diseases including depression, diabetes and heart failure. In addition, insomnia contributes to “substantial economic and societal burden through poor productivity, absence from work, and high health-care costs”. The problem is increasingly evident. However, the solution is much more nebulous if you judge by the difficulty that many people find when searching for an effective and safe solution.
The medical literature is replete with examples of natural remedies and practices that improve sleep quality with minimal side effects. Mind-body approaches are almost always my preferred alternative to drugs when working with a client that is having difficulty sleeping. In my opinion, addressing any underlying mental or psychological contributors to sleeplessness should take precedence over simply popping a supplement or drinking an herbal tea. This is not to say that supplements and teas do not have their place in managing insomnia. In some instances they do, in fact, help to provide temporary relief or work as an adjunct to mind-body practices.
Mindfulness meditation tops my list of mind-body approaches for sleep disturbances that involve anxious feelings and nighttime restlessness. Recent studies indicate that practicing Mindfulness-Based Stress Reduction (MBSR) for as little as 8 weeks lowers stress hormone levels (cortisol) and improves sleep quality significantly. Other clinically validated mind-body techniques include: a) the use of lavender oil aromatherapy prior to and during sleep; b) Tai Chi exercise practiced thrice-weekly; c) acupuncture administered to specific acupoints or meridians that are individually tailored for each patient; d) foot massage (reflexology) and/or “therapeutic massage”. In many instances, these holistic modalities also exact other “side benefits” including a decline in daytime fatigue, menopausal symptoms and pain.
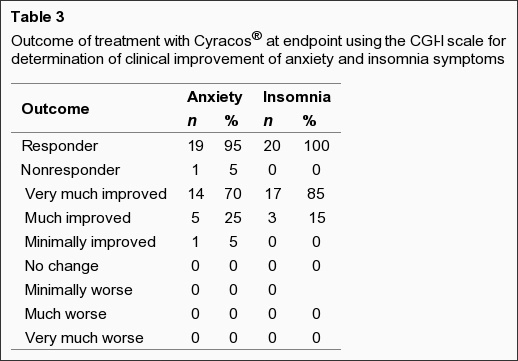
If additional support is called for, several dietary supplements may be particularly useful. One avenue certainly worth pursuing is to test your Vitamin D status. A current study in the journal Acta Paediatrica reports that correcting Vitamin D deficiency can improve mood and sleep difficulties in depressed adolescents. L-theanine, an amino acid commonly found in green tea, can likewise ameliorate objective sleep quality in youngsters with attention deficit hyperactivity disorder (ADHD). A relatively high dosage of 400 mg/day of Suntheanine was used in the aforementioned trial. Finally, a concentrated extract of Melissa officianalis L. or lemon balm was recently shown to quickly lower anxiety and related sleep disturbance in chronically stressed adults. The benefits of lemon balm manifested within 15 days when using 600 mg/day of a patented extract known as Cyracos. Both Cyracos and Suntheanine were deemed safe and well tolerated in the context of these two short term studies.
Note: Please check out the “Comments & Updates” section of this blog – at the bottom of the page. You can find the latest research about this topic there!
To learn more about the studies referenced in today’s column, please click on the following links:
Study 1 – New Research: Identify and Treat Insomnia Early to Reduce Risk of … (link)
Study 2 – Influence of Mindfulness Practice on Cortisol and Sleep in Long-Term … (link)
Study 3 – Effect of Aromatherapy on the Quality of Sleep in Ischemic Heart … (link)
Study 4 – The Effect of Ti Chi Exercise on the Sleep Quality of the Elderly … (link)
Study 5 – Feasibility Study of Acupuncture for Reducing Sleep Disturbances … (link)
Study 6 – Effect of Therapeutic Massage on Insomnia and Climacteric … (link)
Study 7 – Effects of Foot Reflexology on Fatigue, Sleep and Pain: A Systematic … (link)
Study 8 – Depressed Adolescents in a Case-Series Were Low in Vitamin D and … (link)
Study 9 – The Effects of L-Theanine (Suntheanine) on Objective Sleep Quality … (link)
Study 10 – Pilot Trial of Melissa Officinalis L. Leaf Extract in the Treatment of … (link)
Lemon Balm Extract (Cyranos) Improves Sleep Quality
Source: Med J Nutrition Metab. 2011 December; 4(3): 211–218. (link)
Tags: Anxiety, Lavender, Massage
Posted in Alternative Therapies, Mental Health, Nutritional Supplements


March 6th, 2012 at 6:41 pm
I am one who has had pretty bad sleep problems of late, especially because of anxieties about the stresses of daily life! I find that meditation is definitely a good way to relax in the evening in order to improve my chances of getting a good sleep…
March 7th, 2012 at 12:08 am
Thanks for sharing your experience with us, Mark.
We frequently meditate prior to retiring at night. It’s a great way to transition into a restful nights sleep.
Be well!
JP
March 8th, 2012 at 5:06 am
Hiya JP,
great article ☺ Have to add something new and (for me) interesting: Rooibos seems to alleviate stress symptoms by reducing cortisol levels. Seems a perfect relaxing cup of tisane in the evening to calm down ;-))))
http://www.ncbi.nlm.nih.gov/pubmed/22101210
Be well!
Nina K.
March 8th, 2012 at 12:42 pm
Thank you, Nina!
This will remind me to drink more rooibos. I prefer the green, unfermented variety when I can find it. And now, I’ll enjoy it more often whenever I feel stressed. 😉
Be well!
JP
March 15th, 2012 at 7:45 pm
I have had insomnia for over 20 years. I have been on sleeping pills for ever. This past year I have been meditating and practicing Mindfulness as well as hypnosis. I am hoping all or one will start to help me. I have Chronic Fatigue Syndrome so it is hard to figure out what came first the insomnia or the illness.
February 16th, 2015 at 4:56 pm
Update: More support for mindfulness meditation re: sleep quality …
http://archinte.jamanetwork.com/article.aspx?articleid=2110998
Mindfulness Meditation and Improvement in Sleep Quality and Daytime Impairment Among Older Adults With Sleep Disturbances: A Randomized Clinical Trial
Importance: Sleep disturbances are most prevalent among older adults and often go untreated. Treatment options for sleep disturbances remain limited, and there is a need for community-accessible programs that can improve sleep.
Objective: To determine the efficacy of a mind-body medicine intervention, called mindfulness meditation, to promote sleep quality in older adults with moderate sleep disturbances.
Design, Setting, and Participants: Randomized clinical trial with 2 parallel groups conducted from January 1 to December 31, 2012, at a medical research center among an older adult sample (mean [SD] age, 66.3 [7.4] years) with moderate sleep disturbances (Pittsburgh Sleep Quality Index [PSQI] >5).
Interventions: A standardized mindful awareness practices (MAPs) intervention (n = 24) or a sleep hygiene education (SHE) intervention (n = 25) was randomized to participants, who received a 6-week intervention (2 hours per week) with assigned homework.
Main Outcomes and Measures: The study was powered to detect between-group differences in moderate sleep disturbance measured via the PSQI at postintervention. Secondary outcomes pertained to sleep-related daytime impairment and included validated measures of insomnia symptoms, depression, anxiety, stress, and fatigue, as well as inflammatory signaling via nuclear factor (NF)–κB.
Results: Using an intent-to-treat analysis, participants in the MAPs group showed significant improvement relative to those in the SHE group on the PSQI. With the MAPs intervention, the mean (SD) PSQIs were 10.2 (1.7) at baseline and 7.4 (1.9) at postintervention. With the SHE intervention, the mean (SD) PSQIs were 10.2 (1.8) at baseline and 9.1 (2.0) at postintervention. The between-group mean difference was 1.8 (95% CI, 0.6-2.9), with an effect size of 0.89. The MAPs group showed significant improvement relative to the SHE group on secondary health outcomes of insomnia symptoms, depression symptoms, fatigue interference, and fatigue severity (P < .05 for all). Between-group differences were not observed for anxiety, stress, or NF-κB, although NF-κB concentrations significantly declined over time in both groups (P < .05). Conclusions and Relevance: The use of a community-accessible MAPs intervention resulted in improvements in sleep quality at immediate postintervention, which was superior to a highly structured SHE intervention. Formalized mindfulness-based interventions have clinical importance by possibly serving to remediate sleep problems among older adults in the short term, and this effect appears to carry over into reducing sleep-related daytime impairment that has implications for quality of life. Be well! JP
March 12th, 2015 at 1:32 pm
Update: L-Theanine, a component of green tea, improves sleep quality …
http://www.ncbi.nlm.nih.gov/pubmed/25759004
J Am Coll Nutr. 2015 Mar 11:1-12.
In Search of a Safe Natural Sleep Aid.
Sleep deprivation is associated with an elevated risk of various diseases and leads to a poor quality of life and negative socioeconomic consequences. Sleep inducers such as drugs and herbal medicines may often lead to dependence and other side effects. l-Theanine (γ-glutamylethylamide), an amino acid naturally found abundant in tea leaves, has anxiolytic effects via the induction of α brain waves without additive and other side effects associated with conventional sleep inducers. Anxiolysis is required for the initiation of high-quality sleep. In this study, we review the mechanism(s), safety, and efficacy of l-theanine. Collectively, sleep studies based on an actigraph, the obstructive sleep apnea (OSA) sleep inventory questionnaire, wakeup after sleep onset (WASO) and automatic nervous system (ANS) assessment, sympathetic and parasympathetic nerve activities, and a pediatric sleep questionnaire (PSQ) suggest that the administration of 200 mg of l-theanine before bed may support improved sleep quality not by sedation but through anxiolysis. Because l-theanine does not induce daytime drowsiness, it may be useful at any time of the day. The no observable adverse effect level (NOAEL) for the oral administration of l-theanine was determined to be above 2000 mg/kg bw/day. Key teaching points: Sleep deprivation-associated morbidity is an increasing public health concern posing a substantial socioeconomic burden. Chronic sleep disorders may seriously affect quality of life and may be etiological factors in a number of chronic diseases such as depression, obesity, diabetes, and cardiovascular diseases. Most sleep inducers are sedatives and are often associated with addiction and other side effects. l-Theanine promotes relaxation without drowsiness. Unlike conventional sleep inducers, l-theanine is not a sedative but promotes good quality of sleep through anxiolysis. This review suggests that l-theanine is a safe natural sleep aid.
Be well!
JP
April 6th, 2015 at 1:48 pm
Update: Hypnosis improves cognition and sleep in seniors …
http://www.sciencedirect.com/science/article/pii/S0028393215000627
Neuropsychologia Volume 69, March 2015
Improving sleep and cognition by hypnotic suggestion in the elderly
Highlights
• Hypnotic suggestions increase the amount of deep sleep by 57% in the elderly.
• Deeper sleep by hypnosis improves prefrontal cognitive functioning.
• Well-controlled study using high density EEG recordings in the sleep laboratory.
• Hypnosis might have the potential to benefit sleep and cognition in healthy aging.
Abstract
Sleep quality markedly declines across the human lifespan. Particularly the amount of slow-wave sleep (SWS) decreases with age and this decrease is paralleled by a loss of cognitive functioning in the elderly. Here we show in healthy elderly females that the amount of SWS can be extended by a hypnotic suggestion “to sleep deeper” before sleep. In a placebo-controlled cross-over design, participants listened to hypnotic suggestions or a control tape before a midday nap while high density electroencephalography was recorded. After the hypnotic suggestion, we observed a 57% increase in SWS in females suggestible to hypnosis as compared to the control condition. Furthermore, left frontal slow-wave activity (SWA), characteristic for SWS, was significantly increased, followed by a significant improvement in prefrontal cognitive functioning after sleep. Our results suggest that hypnotic suggestions might be a successful alternative for widely-used sleep-enhancing medication to extend SWS and improve cognition in the elderly.
Be well!
JP
April 13th, 2015 at 2:08 pm
Update 4/13/15:
http://medicalxpress.com/news/2015-04-brain-medication-counter-insomnia.html
“People who suffer from sleeplessness, also known as insomnia, are often in a state of ‘hyperarousal’. Resorting to tablets seems to be the obvious solution”, explains the researcher. However, medication-based treatments are usually for short-term use only and confine themselves to fighting this state of arousal, resulting in undesirable side effects including dependence, morningness, drowsiness or amnesia. “Medication often just reduces nocturnal brain activities and thus also helpful functions such as ‘memory consolidation’, which is the nocturnal stabilisation of information so that recall is easier the next day”, says Manuel Schabus. The neurofeedback training deployed within the framework of the FWF project, a type of biofeedback training for the brain, guides the affected persons into sleep. So-called “sleep spindles” are used in this process. These are patterns identified in EEG measurements which are characterised by “spindle-like” rapid rising and falling brain oscillations, and which occur especially during light sleep.”
Study Abstract: http://www.ncbi.nlm.nih.gov/pubmed/23548378
Biol Psychol. 2014 Jan;95:126-34.
Enhancing sleep quality and memory in insomnia using instrumental sensorimotor rhythm conditioning.
EEG recordings over the sensorimotor cortex show a prominent oscillatory pattern in a frequency range between 12 and 15 Hz (sensorimotor rhythm, SMR) under quiet but alert wakefulness. This frequency range is also abundant during sleep, and overlaps with the sleep spindle frequency band. In the present pilot study we tested whether instrumental conditioning of SMR during wakefulness can enhance sleep and cognitive performance in insomnia. Twenty-four subjects with clinical symptoms of primary insomnia were tested in a counterbalanced within-subjects-design. Each patient participated in a SMR- as well as a sham-conditioning training block. Polysomnographic sleep recordings were scheduled before and after the training blocks. Results indicate a significant increase of 12-15 Hz activity over the course of ten SMR training sessions. Concomitantly, the number of awakenings decreased and slow-wave sleep as well as subjective sleep quality increased. Interestingly, SMR-training enhancement was also found to be associated with overnight memory consolidation and sleep spindle changes indicating a beneficial cognitive effect of the SMR training protocol for SMR “responders” (16 out of 24 participants). Although results are promising it has to be concluded that current results are of a preliminary nature and await further proof before SMR-training can be promoted as a non-pharmacological approach for improving sleep quality and memory performance.
Be well!
JP
May 30th, 2015 at 8:33 pm
Update 05/30/15:
http://www.ncbi.nlm.nih.gov/pubmed/26023343
Iran Red Crescent Med J. 2015 Apr 25;17(4):e25880.
Lavender fragrance essential oil and the quality of sleep in postpartum women.
BACKGROUND: Labor and delivery is a stressful stage for mothers. During these periods, sleep-related disorders have been reported. The problems of inadequate sleep include decrease in concentration, judgment, difficulty in performing daily activities, and an increase in irritability. Even the effects of moderate sleep loss on life and health quality can be similar to sleep deprivation. some research aggravated by aromatherapy on sleep quality in different periods of life so might be useful for the improve of sleep quality in postpartum women.
OBJECTIVES: This study aimed to determine the effect of aromatherapy on the quality of sleep in postpartum women. The sample was recruited from medical health centers of Zanjan University of Medical Sciences.
PATIENTS AND METHODS: This study was a randomized clinical trial with the control group. A total of 158 mothers in postpartum period (with certain inclusion criteria) were enrolled in the study and assigned randomly to two groups of control and intervention. Lavender fragrance (made by Barij Essence Pharmaceutical Co.) was used by participants in the intervention group nightly before sleeping. The fragrance was dropped on cotton balls, which were placed on a cylindrical container at mothers’ disposal. Keeping the container at a projected distance of 20 cm, the participants inhaled 10 deep breaths and then the container was placed beside their pillow until morning. This procedure was done 4 times a week for 8 weeks. For the control group, the same intervention was done with the placebo. The instrument for collecting data was Pittsburgh sleep quality index, which was completed at the baseline, fourth, and eighth weeks after the intervention. Data were analyzed using independent t test and repeated measures analysis of variance calculated by SPSS16.
RESULTS: Before the intervention, there were no significant differences between mothers in two groups (P > 0.05). After 8 weeks follow up, a significant improvement appeared in mothers’ sleep quality in the intervention group. Aromatherapy increased sleep quality mean score (±SD) from 8.2911 (± 2.1192) to 6.7975 (± 2.3663) (P < 0.05), but in the control group sleep quality mean score (±SD) changes from 8.4557 (± 2.3027) to 7.5696 (± 1.1464) (P > 0.05). Comparing sleep quality between control and intervention groups after 8 weeks from the beginning of the intervention indicated that aromatherapy was effective in the improvement of mothers’ sleep quality (P < 0.05). CONCLUSIONS: Considering the effects of aromatherapy on the improvement of mother's sleep quality during postpartum period, aromatherapy has been suggested as a non-pharmacological method for the improvement of the maternal health. Be well! JP
July 14th, 2015 at 2:45 pm
Update 07/14/15:
http://www.ncbi.nlm.nih.gov/pubmed/26158889
Sleep. 2015 Jun 22.
Efficacy of Cognitive Behavioral Therapy for Insomnia in Adolescents: A Randomized Controlled Trial with Internet Therapy, Group Therapy and a Waiting List Condition.
STUDY OBJECTIVES: To investigate the efficacy of cognitive behavioral therapy for insomnia (CBTI) in adolescents.
DESIGN: A randomized controlled trial of CBTI in group therapy (GT), guided internet therapy (IT), and a waiting list (WL), with assessments at baseline, directly after treatment (post-test), and at 2 months follow-up.
SETTING: Diagnostic interviews were held at the laboratory of the Research Institute of Child Development and Education at the University of Amsterdam. Treatment for GT occurred at the mental health care center UvAMinds in Amsterdam, the Netherlands.
PARTICIPANTS: One hundred sixteen adolescents (mean age = 15.6 y, SD = 1.6 y, 25% males) meeting DSM-IV criteria for insomnia, were randomized to IT, GT, or WL.
INTERVENTIONS: CBTI of 6 weekly sessions, consisted of psychoeducation, sleep hygiene, restriction of time in bed, stimulus control, cognitive therapy, and relaxation techniques. GT was conducted in groups of 6 to 8 adolescents, guided by 2 trained sleep therapists. IT was applied through an online guided self-help website with programmed instructions and written feedback from a trained sleep therapist.
MEASUREMENTS AND RESULTS: Sleep was measured with actigraphy and sleep logs for 7 consecutive days. Symptoms of insomnia and chronic sleep reduction were measured with questionnaires. Results showed that adolescents in both IT and GT, compared to WL, improved significantly on sleep efficiency, sleep onset latency, wake after sleep onset, and total sleep time at post-test, and improvements were maintained at follow-up. Most of these improvements were found in both objective and subjective measures. Furthermore, insomnia complaints and symptoms of chronic sleep reduction also decreased significantly in both treatment conditions compared to WL. Effect sizes for improvements ranged from medium to large. A greater proportion of participants from the treatment conditions showed high end-state functioning and clinically significant improvement after treatment and at follow-up compared to WL.
CONCLUSIONS: This study is the first RCT that provides evidence that CBTI is effective for the treatment of adolescents with insomnia, with medium to large effect sizes. There were small differences between internet- and group therapy, but both treatments reached comparable endpoints.
Be well!
JP
July 28th, 2015 at 11:19 am
Updated 07/28/15:
http://www.ncbi.nlm.nih.gov/pubmed/26211735
Nurs Crit Care. 2015 Jul 27.
Effects of aromatherapy on sleep quality and anxiety of patients.
BACKGROUND: In intensive care units (ICUs), patients cannot sleep well. Aromatherapy is used for depression, anxiety, relaxation and disorders related with sleep and stress.
AIM: This study aimed to investigate the effect of lavender essential oil on the sleep quality and anxiety level of patients in coronary ICU.
PARTICIPANTS: A total of 60 patients in coronary ICU participated in this study.
DESIGN: A randomized controlled study was conducted with 60 patients in a province located in the southeast of Turkey.
METHODS: After informing the patients in both groups about the study, they were administered a questionnaire, Pittsburgh Sleep Quality Index (PSQI) and the Beck Anxiety Inventory (BAI) scale. The patients in the intervention group were given 2% lavender essential oil via inhalation for 15 days after which they were administered the same scales again to evaluate the sleep quality and anxiety. As for the control group, they were administered the same scales again after 15 days without the inhalation of lavender essential oil.
RESULTS: Comparison of the PSQI and BAI scores of the patients in the control and intervention groups before and after the intervention showed statistically significant differences in the change in favour of the intervention group (p < 0·05). CONCLUSION: Lavender essential oil increased quality of sleep and reduced level of anxiety in patients with coronary artery disease. RELEVANCE TO CLINICAL PRACTICE: As a non-invasive, cheap, easily applicable, cost-effective, independent nursing intervention and appropriate for cardiac patients, lavender essential oil could be applied in ICUs. Be well! JP
December 17th, 2015 at 11:55 pm
Updated 12/17/15:
http://online.liebertpub.com/doi/10.1089/acm.2015.0018
J Altern Complement Med. 2015 Dec 15.
Effects of Ayurvedic Oil-Dripping Treatment with Sesame Oil vs. with Warm Water on Sleep: A Randomized Single-Blinded Crossover Pilot Study.
OBJECTIVES: Ayurvedic oil-dripping treatment (Shirodhara) is often used for treating sleep problems. However, few properly designed studies have been conducted, and the quantitative effect of Shirodhara is unclear. This study sought to quantitatively evaluate the effect of sesame oil Shirodhara (SOS) against warm water Shirodhara (WWS) on improving sleep quality and quality of life (QOL) among persons reporting sleep problems.
METHODS: This randomized, single-blinded, crossover study recruited 20 participants. Each participant received seven 30-minute sessions within 2 weeks with either liquid. The washout period was at least 2 months. The Shirodhara procedure was conducted by a robotic oil-drip system. The outcomes were assessed by the Pittsburgh Sleep Quality Index (PSQI) for sleep quality, Epworth Sleepiness Scale (ESS) for daytime sleepiness, World Health Organization Quality of Life 26 (WHO-QOL26) for QOL, and a sleep monitor instrument for objective sleep measures. Changes between baseline and follow-up periods were compared between the two types of Shirodhara. Analysis was performed with generalized estimating equations.
RESULTS: Of 20 participants, 15 completed the study. SOS improved sleep quality, as measured by PSQI. The SOS score was 1.83 points lower (95% confidence interval [CI], -3.37 to -0.30) at 2-week follow-up and 1.73 points lower (95% CI, -3.84 to 0.38) than WWS at 6-week follow-up. Although marginally significant, SOS also improved QOL by 0.22 points at 2-week follow-up and 0.19 points at 6-week follow-up compared with WWS. After SOS, no beneficial effects were observed on daytime sleepiness or objective sleep measures.
CONCLUSIONS: This pilot study demonstrated that SOS may be a safe potential treatment to improve sleep quality and QOL in persons with sleep problems.
Be well!
JP
April 15th, 2016 at 10:10 am
Updated 04/15/16:
http://www.ncbi.nlm.nih.gov/pubmed/27078810
Holist Nurs Pract. 2016 May-Jun;30(3):155-165.
Assessment of Sleep Quality and Effects of Relaxation Exercise on Sleep Quality in Patients Hospitalized in Internal Medicine Services in a University Hospital: The Effect of Relaxation Exercises in Patients Hospitalized.
This study aims to assess sleep quality and determine the effects of relaxation exercise on sleep quality in patients hospitalized in internal medicine services. In total, 47 patients comprised the control group and did not engage in the exercise intervention-the progressive muscle relaxation exercise, whereas 235 patients were assigned to the intervention group (N = 282). In this study, Description Questionnaire Form and the Pittsburg Sleep Quality Index (PSQI) were used. Most patients (73.8%) had poor sleep quality. The mean pre- and postexercise PSQI scores of the patients in the interventional group were 8.7 ± 4.0 and 6.1 ± 3.3, respectively. The mean pre- and postexercise PSQI scores of the control patients were 6.6 ± 3.5 and 5.6 ± 2.7, respectively. According to this study, the exercises significantly enhanced the quality of sleep. Patients should be encouraged by nurses to perform relaxation exercises.
Be well!
JP
June 13th, 2017 at 11:50 am
Updated 06/13/17:
https://www.ncbi.nlm.nih.gov/pubmed/28603433
Nat Sci Sleep. 2017 May 26;9:163-169.
Evaluation of effectiveness and safety of a herbal compound in primary insomnia symptoms and sleep disturbances not related to medical or psychiatric causes.
BACKGROUND AND PURPOSE: Sleep disturbances and related daytime activities impairment are common diseases nowadays. General practitioners are often the first health care professional asked to alleviate sleep disturbances and primary insomnia symptoms. Beyond a wide class of hypnotic drugs, botanicals can represent an alternative treatment for those kinds of symptoms. The scope of the present study is to evaluate safety and effectiveness of a herbal compound composed of valerian, hop, and jujube (Vagonotte®) on primary insomnia symptoms and sleep disturbances not related to medical or psychiatric causes.
PATIENTS AND METHODS: One hundred and twenty subjects with sleep disturbances symptoms were randomized in two branches of 60 persons each, receiving the herbal compound or placebo at dosage of two pills per day 30 minutes before their scheduled bedtime. All subjects were screened for precise items related to sleep quality and daytime activity at the beginning, after 10 days, and after 20 days of consecutive dietary supplement (or placebo) consumption. The participants remained blind to group assignment until all of them completed the trial.
RESULTS: Sleep onset, numbers of nocturnal awakenings, and overall nocturnal slept time were assessed. A statistically significant difference between the two groups emerged. The group receiving the herbal compound showed a lower time of sleep onset compared to placebo group, the same result was obtained for total slept time and night awakenings frequency (p<0.001). Daily symptom improvement in subjects receiving the herbal compound showed significant reduction in tension and irritability, difficulty in concentration, and fatigue intensity, if compared to placebo scores (p<0.001). None of the 60 subjects in the verum group reported adverse reaction related to the herbal compound, and 98% of subjects judged the product as having from good to excellent safety and tolerability.
CONCLUSION: Botanicals dietary supplement with relaxing and soothing properties can help practitioner to treat primary insomnia, especially when the risk/benefit profile of a patient does not sustain hypnotic drugs prescription. This clinical investigation on safety and effectiveness of a herbal compound made of valerian, hop, and jujube opens interesting perspectives on usage of herbal compound to manage primary insomnia. Further investigations could help in understanding herbal compounds' effectiveness on sleep disturbances.
Be well!
JP
October 7th, 2017 at 1:59 pm
Updated 10/07/17:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5612039/
Sleep Sci. 2017 Apr-Jun;10(2):68-72.
Effect of yoga and aerobics exercise on sleep quality in women with Type 2 diabetes: a randomized controlled trial.
OBJECTIVE: The aim of this study was investigating the effect of 12 weeks of yoga and aerobic exercise (running on a treadmill) on the sleep quality in women with Type 2 diabetes.
MATERIALS AND METHODS: 39 diabetic women were selected from Semnan city with the mean age of 46.85±3.35 years, weight of 69.79±17.18 kg, height of 155.03±5.00, BMI of 29.64±5.00 kg/m2 who had a background of diabetes for 6.46±2.69 years. They were then randomly divided into yoga exercise (n=15), aerobic exercise (n=13), and control group (n=11). The exercise program was performed for 12 weeks, three sessions per each week. In order to measure the sleep quality, the Pittsburgh Sleep Quality Index (PSQI) was used. The data were analyzed by non-parametric wilcoxon and Kruskal-Wallis Test at significance level of p<0.05.
RESULTS: Overall score of sleep quality improved after six (p=0.001) and 12 (p=0.001) weeks of yoga exercise. Also, significant effect was observed after 6 weeks of aerobic exercise (p=0.039). However, the positive effect was diminished to under significant levels after 12 weeks of aerobic exercise (p=0.154). Kruskal-Wallis Test showed significant differences between yoga and aerobic groups after 12 weeks of exercise (p=0.002). No significant differences were observed in control groups in all situation.
CONCLUSIONS: It can be concluded that yoga exercise is more effective in improving the sleep quality in comparison with the same course of aerobic exercise in women suffering from diabetes Type 2. Thus, yoga exercise can be suggested to these patients.
Be well!
JP
December 6th, 2017 at 5:47 pm
Updated 12/06/17:
https://www.jstage.jst.go.jp/article/jcbn/61/3/61_17-6/_pdf/-char/en
J Clin Biochem Nutr. 2017 Nov;61(3):210-216.
Ingestion of green tea with lowered caffeine improves sleep quality of the elderly via suppression of stress.
Epidemiological and animal studies have demonstrated that ingestion of green tea enhances healthy life. However, caffeine in green tea can interfere with sleep. In this report, we examined the effect of green tea with lowered caffeine, low-caffeine green tea, on stress and sleep of the elderly. The participants (n = 10, mean age 89.3 ± 4.2 years) drank five cups/day of standard green tea for 1 week. Subsequently, they drank five cups/day of low-caffeine green tea for 2 weeks. Salivary α-amylase activity (sAA) was measured as a stress marker. Sleep stages were measured using a portable electroencephalography (n = 7, 6 female and 1 male). The level of sAA in the morning (sAAm) was significantly lower when the participants drank low-caffeine green tea than standard green tea. While the levels of sAAm were different among individuals, lower sAAm correlated with a higher quality of sleep. In those participants whose sAAm was lowered by the ingestion of low-caffeine green tea, some sleep parameters improved. Daily ingestion of low-caffeine green tea may be a beneficial tool for improving the quality of sleep of the elderly via the suppression of stress, although further research is required to fortify this hypothesis.
Be well!
JP
December 9th, 2017 at 11:13 pm
Updated 12/09/17:
https://www.ncbi.nlm.nih.gov/pubmed/29217495
J Ethnopharmacol. 2017 Dec 4.
Efficacy of Violet oil, a Traditional Iranian Formula, in Patients with Chronic Insomnia: A Randomized, Double-Blind, Placebo-Controlled Study.
ETHNOPHARMACOLOGICAL RELEVANCE: Violet oil is an ancient herbal drug which has been extensively used to treat insomnia in traditional Iranian Medicine clinics. Violet oil is an almond or sesame oil-based extract of Viola odorata, which is administered as nasal drops. This study aimed to evaluate the efficacy of Violet oil in the treatment of insomnia.
METHODS AND MATERIALS: This study was conducted as a 3-arm double-blind randomized trial. A total of 75 patients with chronic insomnia were enrolled and randomly assigned to three groups in Traditional Iranian Medicine Clinic of Mashhad University of Medical Sciences, Mashhad, Iran. The treatment consisted of intranasal dropping of Violet oil, Almond oil or placebo (1% solution of Carboxymethyl cellulose) in each nostril every night before sleep for 30 days, i.e. three drops of the drug (including either Violet oil or Almond oil) or the placebo was used every night before the sleep. All the patients were asked to complete Pittsburgh Sleep Quality Index (PSQI) and Insomnia Severity Index (ISI) questionnaires before and after the intervention.
RESULTS: There were no significant differences between patients in the three groups before the intervention (P > 0.05). However, there were significant differences between the three groups after the intervention in ISI scores (P<0.002) and PSQI scores (p<0.001). When comparing the pre- and post-treatment data, the ISI and PSQI scores improved significantly in all the three groups as follows: Violet oil (P<0.001), Almond oil (P<0.001) and placebo (P<0.001). The results also showed that the Violet oil had the most effect among the three groups. In addition, it was more effective on sleep quality than sleep quantity.
CONCLUSION: Considering the effects of natural nasal drug on the improvement of sleep quality in insomniac patients, this study has proposed the use of Violet oil as a natural and herbal drug in a non-oral method without serious side effects for treatment of insomnia.
Be well!
JP
December 14th, 2017 at 2:38 pm
Updated 12/14/17:
https://www.ncbi.nlm.nih.gov/pubmed/29234416
Evid Based Complement Alternat Med. 2017;2017:6419439.
Effects of Bedtime Periocular Warming on Sleep Status in Adult Female Subjects: A Pilot Study.
Several studies have reported that suitable manipulation of human skin or body temperature can lead to improved sleep. To clarify the effect of skin warming on human sleep, 38 female subjects, who occasionally had difficulty with falling asleep, were studied. The participants underwent two experimental sessions, which were carried out in two consecutive follicular phases and randomly crossed over. The participants wore hot or sham eye masks in one 14-day session. The first half of each 14-day session was designated the baseline period (BL) without any interventions and the later half was designated the intervention period (INT), in which they wore either the hot or sham eye mask for 10 minutes at bedtime. All the participants were instructed to keep a sleep diary every morning for the BL and INT. The results showed that the hot eye mask was significantly preferred over the sham one with respect to comfort and that feelings of restfulness and being refreshed upon wakening in the morning were significantly better with the hot eye mask than with the sham. These results suggest that bedtime periocular warming has favorable effects on subjective well-being on awakening, possibly due to the sense of comfort experienced at bedtime.
Be well!
JP
January 10th, 2018 at 2:32 pm
Updated 1/10/18:
http://journals.lww.com/jnr-twna/Abstract/publishahead/Effects_of_Auricular_Acupressure_on_Sleep_Quality,.99889.aspx
J Nurs Res. 2018 Feb;26(1):10-17.
Effects of Auricular Acupressure on Sleep Quality, Anxiety, and Depressed Mood in RN-BSN Students With Sleep Disturbance.
BACKGROUND: Students in 2-year registered nurse to Bachelor of Science in nursing (RN-BSN) programs usually work full-time and study part-time. Sleep disturbance, anxiety, and depression are known to be common health problems among these students.Prior research has described the effectiveness of auricular acupressure (AA) in reducing sleep disturbance and improving mood.
PURPOSE: The aim of this study was to evaluate the effect of using a 4-week AA program that adheres to a magnetic pellet on the shenmen acupoint on sleep quality, anxiousness, and depressed moods in nursing students with sleep disturbance.
METHODS: This study used a one-group, quasi-experimental design with repeated measures. Eligible students were recruited from an RN-BSN program offered by a university in northern Taiwan, and all were currently experiencing sleep disturbance. A 4-week AA intervention that applied a magnetic pellet on the shenmen acupoint was used. The Pittsburgh Sleep Quality Index, Beck Anxiety Inventory, and Beck Depression Inventory-II were used to measure sleep quality and mood outcomes each week during the 4-week intervention. Improvements in sleep quality, anxiety, and depressed moods were analyzed using the generalized estimating equation.
RESULTS: Thirty-six participants with a mean age of 32 years were enrolled as participants. After adjusting for confounding factors, continuous and significant improvements in sleep quality, anxiety, and depressed mood (p < .05) were observed throughout the intervention, with 4-week improvements in sleep quality, anxiety, and depressed mood averaging 26.7%, 43.5%, and 25%, respectively. CONCLUSIONS/IMPLICATIONS FOR PRACTICE: This study showed the efficacy of using a 4-week AA that applies a magnetic pellet on the shenmen acupoint in terms of improving sleep quality, anxiousness, and depressed mood in RN-BSN students experiencing sleep disturbances. Especially, the emotional mood of participants improved significantly as early as the first week. The 4-week AA for reducing sleep disturbance, and improving students' anxiety, and depressed moods may be applied on primary healthcare. Be well! JP
February 19th, 2018 at 2:28 pm
Updated 2/19/18:
http://www.ijoy.org.in/article.asp?issn=0973-6131;year=2017;volume=10;issue=3;spage=128;epage=137;aulast=Rshikesan
Int J Yoga. 2017 Sep-Dec;10(3):128-137.
Sleep Quality and Body Composition Variations in Obese Male Adults after 14 Weeks of Yoga Intervention: A Randomized Controlled Trial.
Background: Obesity is a big challenge all over the world. It is associated with many noncommunicable diseases. Yoga known to be add-on treatment may be effective for obesity control.
Aim: To assess the effect of integrated approach of yoga therapy (IAYT) for body composition and quality of sleep in adult obese male.
Subjects and Methods: A randomized controlled trial was conducted for 14 weeks on obese male of urban setting. Eighty individuals were randomly divided into two groups, i.e., yoga group (n = 40; age; 40.03 ± 8.74 years, body mass index [BMI] 28.7 ± 2.35 kg/m2) and control group (age; 42.20 ± 12.06 years, BMI 27.70 ± 2.05 kg/m2). The IAYT was imparted to yoga group for 1½ hour for 5 days in a week for 14 weeks. The control group continued their regular activities. The body composition by InBody R20 and sleep quality by Pittsburgh Sleep Quality Index (PSQI) were assessed. Statistical analysis was done for within and between groups using SPSS version 21. The correlation analysis was done on the difference in pre-post values.
Results: The results showed that weight (P = 0.004), BMI (P = 0.008), bone mass (P = 0.017), obesity degree (P = 0.005), and mineral mass (P = 0.046) were improved in yoga group and no change in control group (P > 0.05). The global score of PSQI improved (P = 0.017) in yoga group alone.
Conclusion: The results indicate the beneficial effects of IAYT on body composition and sleep quality in obese males. The yoga practice may reduce obesity with the improvement in quality of life.
Be well!
JP
May 2nd, 2018 at 6:49 pm
Updated 05/01/18:
https://www.ncbi.nlm.nih.gov/pubmed/29705482
Complement Ther Clin Pract. 2018 May;31:64-70.
The effect of progressive muscle relaxation on the management of fatigue and quality of sleep in patients with chronic obstructive pulmonary disease: A randomized controlled clinical trial.
OBJECTIVE: To assess the effect of progressive muscle relaxation (PMR) on fatigue and sleep quality of patients with chronic obstructive pulmonary disease (COPD) stages 3 and 4.
MATERIALS AND METHODS: The pretest posttest clinical trial recruited 91 patients COPD grades 3 and 4. Following random assignment of subjects, the treatment group (n = 45) performed PMR for eight weeks and the control group (n = 46) received routine cares. At baseline and after the intervention, fatigue and sleep quality was assessed. Data obtained were analyzed in SPSS.
RESULTS: It was determined that PMR decreased patients’ fatigue level and improved some sleep quality subscales including subjective sleep quality, sleep latency, sleep duration and habitual sleep efficiency, but no improvement was found in global sleep quality and other sleep subscales.
CONCLUSION: An eight-week home-based PMR program can be effective in reducing fatigue and improving certain subscales of sleep quality in patients with COPD stages 3,4.
Be well!
JP
November 29th, 2018 at 2:54 pm
Updated 11/28/18:
https://www.ncbi.nlm.nih.gov/pubmed/30477841
Complement Ther Med. 2018 Dec;41:208-214.
Efficacy of exercise as a treatment for Obstructive Sleep Apnea Syndrome: A systematic review.
INTRODUCTION: Obstructive Sleep Apnea Syndrome (OSAS) is a prevalent condition associated with numerous adverse health consequences. Exercise therapy was described as a valuable OSAS treatment alternative to continuous positive airway pressure.
OBJECTIVE: The objective of the present systematic review was to assess the efficacy of exercise in reducing OSAS severity and associated comorbidities.
SETTING: We queried MEDLINE and SCOPUS and ScienceDirect databases with the following keywords: “sleep apnea” and “sleep disordered breathing” for the population and “physical activity”, “fitness” and “exercise” for the intervention.
RESULTS: Eight studies including a total number of 354 patients showed that OSAS severity was significantly reduced after intervention. This reduction was associated with significant improvement in cardio-vascular fitness, sleep quality and quality of life. Conversely, this effect was not directly related to body weight reduction.
CONCLUSION: This systematic review suggests that physical activity should be recommended as a treatment for OSAS patients. However, further research is necessary to demonstrate this long-term efficiency with a higher level of confidence and to better understand the underlying physiological mechanisms.
Be well!
JP
January 6th, 2019 at 5:08 pm
Updated 01/06/19:
https://clinicalnutritionespen.com/article/S2405-4577(18)30306-1/fulltext
Clin Nutr ESPEN. 2018 Dec;28:132-135.
Effect of milk-honey mixture on the sleep quality of coronary patients: A clinical trial study.
BACKGROUND: Admission of patients in coronary care units can lead to sleep disorders due to advanced monitoring and interventions. Inappropriate sleep quality in cardiac patients may be influenced by their health status. So, this study was performed to detect the effect of Milk-honey mixture on sleep status of acute coronary syndrome patients in the coronary care unit.
METHODS: A clinical trial study (registered under IRCT.ir with identifier no. IRCT201309285134N7) was conducted with 68 hospitalized patients with the acute coronary syndrome in the coronary care unit of a referral hospital in Semnan, Iran. After hospitalization of patients and selected eligible patients, sleep status of them was measured by Richards-Campbell Sleep Questionnaire in range of 0 to 100 score. Then patients were divided into the intervention and control groups randomly. Patients in the intervention group were received milk-honey mixture twice a day for three days. The control group patients were received routine care. In the third day, sleep quality of patients in the two groups was measured again. Finally, the data were analyzed by descriptive and inferential statistics.
RESULTS: The mean and standard deviation of patients’ age was 63.12 ± 32.63. There was no significant difference in sleep scores on the first day of admission between the two groups (P = 0.914). But, on the third day of admission, there was a significant difference in sleep scores between the intervention and the control groups (P = 0.001).
CONCLUSION: The mixture of milk and honey improves the sleep status of patients. So, it can be considered as an effective and affordable intervention to enhance the sleep quality of patients with the acute coronary syndrome in coronary care units.
Be well!
JP
February 16th, 2019 at 4:16 pm
Updated 02/16/19:
https://www.ncbi.nlm.nih.gov/pubmed/30768439
Holist Nurs Pract. 2019 Feb 12.
Effects of Kefir on Quality of Life and Sleep Disturbances in Postmenopausal Women.
The aim of this study is to identify the effects of kefir, an alternative treatment method, on quality of life and sleep disturbances in postmenopausal women. In this study, it is seen that kefir has positive effects on sleep disturbances, depression, and quality of life in postmenopausal women.
Be well!
JP