Preventive Medicine
February 3, 2010 Written by JP [Font too small?]The term “alternative medicine” can be somewhat misleading. If you combine it with the word “complementary”, as in “alternative and complementary medicine”, the meaning becomes considerably more accurate. But even that string of words doesn’t fully convey the essence of holistic healing. The missing link can be summed up in three syllables: pre-ven-tive. It doesn’t sound very snappy, but the phrase “alternative, complementary and preventive medicine” does a fine job of encompassing what natural healing is all about.

It’s very difficult to witness suffering in others. This discomfort is even more pronounced when the people affected are relatively helpless. I know that my own heart breaks when I see children or senior citizens who aren’t receiving the best possible care. These painful instances epitomize why preventive medicine is at the top of the holistic food chain. Simply put, healthy lifestyle choices can and should span the course of a lifetime. Making the right decisions can encourage the wellness of babies in the womb and afford protection against the worst aspects of aging as well.
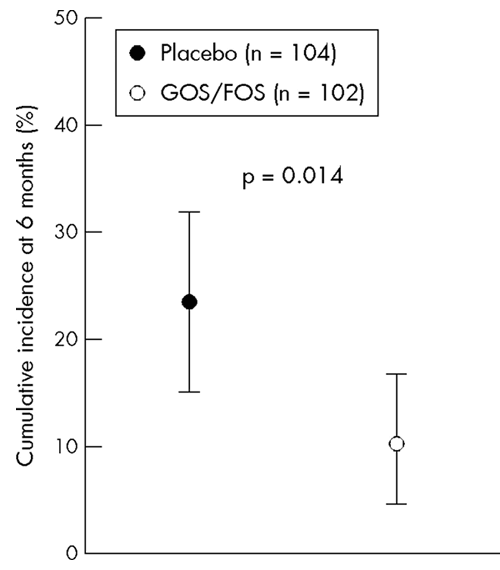
Atopic dermatitis or eczema is an inflammatory skin condition that is quite common among infants and young children. Two new studies suggest that diet may often be a determining factor as to which kids are forced to cope with it. The January 22nd edition of the journal Allergy examined the food selection of 763 “mother-child pairs” in order to investigate any possible connection between diet, supplementation and prevalence of eczema. The Japanese researchers overseeing the trial discovered that higher intakes of beta-carotene, citrus fruit and green + yellow vegetables dramatically lowered the incidence of eczema by 48%, 47% and 59% respectively. Unfortunately, not every mother-to-be eats a diet quite like this. The good news is that similar benefits can be found if young children are fed a comparable diet. A recent study of 422 children revealed that those with the highest blood levels of beta carotene, Vitamin E, folic acid and iron were 50-70% less likely to suffer from eczema. The authors of this second trial commented that, “higher antioxidant nutritional status reduces the risk of AD (atopic dermatitis) and that such risk-reduction effects depend on nutrient type”. (1,2,3)
I was also pleasantly surprised to find a recent German review about the role that diet plays in acne occurrence. The report specifically calls out several foods which tend to promote excessive release of insulin in the body. Here are a few of the key points made in the summary: 1) “Insulinotropic foods, especially milk, dairy products and carbohydrates with high glycemic index and smoking lead to pathological exaggeration of already physiologically increased growth factor signaling of puberty”; 2) “acne is the visible metabolic syndrome of skin exaggerated by growth factor signaling of westernized malnutrition” and; 3) the lead researcher goes as far as to suggest that acne vulgaris should be renamed “acne alimentaris” due to the profound link between poor nutrition and skin problems in adolescents.
Many scientists are cautiously expressing optimism about a proposed link between Vitamin D and the prevention and management of autoimmune diseases such as multiple sclerosis. The latest hopeful sign of this arena can be found in the current issue of the Annals of Neurology. Blood samples were taken from 110 young MS patients over the course of approximately 1.7 years. At the beginning of the study, all of the participants were under the age of 18. Supervising physicians took note of the frequency and severity of MS-related relapses that each volunteer experienced. The results indicate that there was a 34% reduced risk of relapses for every 10 ng/mL increase in Vitamin D levels. In other words, a patient with a Vitamin D level of 20 ng/mL would have a 34% greater relapse risk than a similar patient with a D level of 30 ng/mL. The primary author of the study, Dr. Ellen M. Mowry, summarized the findings in this way: “Although we do not yet know if Vitamin D supplementation will be beneficial for MS patients, the fact that there is a clear association between Vitamin D levels and relapse rate provides a strong rationale for conducting a clinical trial to measure the potential impact of supplementation”. (4,5)
Two other MS/Vitamin D related studies were published in the past few months: the first trial reports that higher serum Vitamin D (25-OH D) may be linked to lower levels of a substance known as IgG (immunoglobulin G), a marker of MS activity. A separate article in the December issue of the Journal of the Neurological Sciences comments on the potential role of Vitamin D in protecting against MS-related bone loss due to the use of glucocorticoid medications. (6,7)
The previous research mostly focused on prevention or subsequent interventions. Now let’s turn to the alternative and complementary side of the holistic equation. Acupuncture is a widely utilized Eastern therapy that can sometimes replace conventional care – this represents the truest sense of an alternative. However in many instances it’s also used as a complementary treatment that may improve outcomes and minimize side effects typically associated with standard care.
Three new studies have examined the potential of acupuncture with regard to women’s health. One of the trials followed 92 young women (14-25 years old) suffering from menstrual pain over the course of one year. During that time, half of the women received 3 months of acupuncture – a total of 9 treatments. At the 3 month mark, those receiving acupuncture reported lower pain scores and “a small reduction in mood changes”. After 6 months, the acupuncture group noted “a significant reduction in the duration of menstrual pain” and required fewer pain relievers to cope with said symptoms. In addition, there were no safety issues documented in relation to the acupuncture treatment and it was deemed “acceptable” by those receiving it. (8)
Minimizing the use of synthetic medications during pregnancy is generally considered desirable by both allopathic and holistically-minded physicians. A Swedish investigation postulates that acupuncture may be a viable alternative to conventional analgesic drugs in pregnant women suffering from low back and pelvic pain. This suggestion is based on a study that was conducted on 40 expectant mothers who received 6 weeks of acupuncture treatment – 8 thirty-minutes sessions in all. It’s interesting to note that half of the participants began treatment at the 20th week of gestation and the remainder started at week 26. Both groups demonstrated significant pain relief and an improvement in quality of life. (9)
Finally, the January 25th edition of the Journal of Clinical Oncology provides an example of using acupuncture in a complementary fashion. 38 women undergoing breast cancer treatment were assigned to “true acupuncture” or sham acupuncture to determine whether either modality might reduce treatment-related joint pain. The true form of acupuncture involved site-specific treatment whereas the sham variety placed needles in “nonacupoint locations”. All of the women received twice-weekly acupuncture for 6 weeks. The participants receiving the true form of acupuncture reported reduced “pain-related interference” and pain severity as quantified by an index known as the Brief Pain Inventory-Short Form. Both forms of acupuncture were well tolerated. The researchers concluded that the women treated with true acupuncture “had significant improvement in joint pain and stiffness, which was not seen with sham acupuncture”. This finding indicates that acupuncture may facilitate a more tolerable experience for breast cancer patients and possibly reduce the number of women who would normally discontinue conventional treatment. (10)
There is a hierarchy by which many holistic practitioners view alternative, complementary and preventive medicine. Prevention is the undisputed king. Historically or scientifically proven alternatives are a distant second and complementary practices are the final resort. The reason for this order is that prevention provides a foundational, long-term approach to wellness. It’s proactive not reactive. The need for alternative remedies often arises because a dedicated and personalized approach to wellness isn’t fully in place. But none of us is perfect and we live in a world that’s littered with plenty of pitfalls. Therefore, there is a real need for alternative “medicines” at times. However, they should be employed much like conventional medications: a) try not to depend on them; b) use them judiciously and only as needed. Finally, in the event that one absolutely requires an allopathic/conventional intervention (prescription medications, surgery, etc.), they should also look into the possibility of supporting that treatment with complementary therapies from the natural side of the healing spectrum.
Be well!
JP
Tags: Acne, Acupuncture, Eczema, Multiple Sclerosis
Posted in Alternative Therapies, Children's Health, Nutrition

February 4th, 2010 at 1:03 am
Thank you for this extra~informative post, HealthyFellow~!
I have a young student who has had some trouble w/ eczema
conditions, & I will be sharing this information with her
mom [whom I’ve talked to somewhat extensively with about
this issue, etc.]
Appreciate you ~!
February 4th, 2010 at 1:16 am
Thank you, Mia B! 🙂
Good on you for getting involved in that way! I sincerely hope your student’s mom is receptive to the information. I know from prior experience that eczema can be quite difficult to live with.
Be well!
JP
February 4th, 2010 at 12:23 pm
Good Day JP 🙂
Acupuncture is really a good recommendation, our health insurance pays that fully – they see it as evidence based medicine. good luck for us. despite the needles its very safe and without side effects and it helps against a wide variety of symptoms.
Stay healthy!
Nina K.
February 4th, 2010 at 12:25 pm
Once again, it all seems to go back to fueling our bodies properly… Awesome article, JP!
~Angie
February 4th, 2010 at 4:36 pm
Thank you, Nina! 🙂
Acupuncture is rarely covered by health insurance here in the states. I’m hoping that will soon change – especially in instances where there’s high quality evidence to supports it’s inclusion into the mainstream.
Be well!
JP
February 4th, 2010 at 4:38 pm
Thanks, Angie! 🙂
Be well!
JP
March 25th, 2015 at 1:37 pm
Update: Natural topical preparations can also reduce eczema symptoms …
Clin Cosmet Investig Dermatol. 2014 Nov 11;7:321-7.
A cosmeceutical formulation based on boswellic acids for the treatment of erythematous eczema and psoriasis.
BACKGROUND: Boswellic acids (BAs) show anti-inflammatory properties in a variety of inflammatory diseases, including rheumatoid arthritis, osteoarthritis, and asthma. A topical administration route is currently used to deliver active compounds in psoriatic and eczematous patients. In this double-blind study we compare a novel BA formulation (containing Bosexil(®), INCI [International Nomenclature of Cosmetic Ingredients]: lecithin, Boswellia serrata resin extract) with a placebo formulation. A third arm of the trial received a formulation of Vaccinium myrtillus seed oil, previously demonstrated as an effective local treatment for psoriatic lesions.
METHODS: Patients with psoriasis or erythematous eczema were randomly assigned, in a 1:1:1 ratio, to Bosexil(®), V. myrtillus seed oil, or placebo. In order to evaluate the effects of treatment, the changes of scales and erythema from diagnosis to the end of treatment were scored in psoriatic patients, while changes in itch and erythema were analyzed for erythematous eczema patients. Psoriasis Area Severity Index and Eczema Area and Severity Index scores were also calculated.
RESULTS: In patients with psoriasis, scales and erythema improved both with Bosexil(®) and the V. myrtillus seed oil treatment in comparison with placebo. In particular, the treatment with Bosexil(®) formulation improved scales (70% of cases) and erythema (50% of cases) without any case of worsening. In patients with eczema, the administration of placebo did not result in any improvement in 90% of cases, and in the remaining 10% worsened both itch and erythema. Bosexil(®) formulation improved both itch (60% of cases) and erythema (60% of cases) without any case of worsening. V. myrtillus seed oil improved itch and erythema in 66.7% and 77.8% of patients, respectively.
CONCLUSION: A topical formulation of Bosexil(®) may be promising for the treatment of psoriasis and erythematous eczema. Long-term studies are recommended to evaluate the adherence to this topical treatment and its clinical benefits in real life.
Be well!
JP
May 6th, 2015 at 3:47 pm
Update 05/06/15:
https://www.thieme-connect.com/DOI/DOI?10.1055/s-0035-1548835
Horm Metab Res. 2015 May 4.
Effects of High-Dose Vitamin D Supplementation on Metabolic Status and Pregnancy Outcomes in Pregnant Women at Risk for Pre-Eclampsia.
This study was designed to assess the beneficial effects of high-dose (cholecalciferol) vitamin D supplementation on metabolic profiles and pregnancy outcomes among pregnant women at risk for pre-eclampsia. This randomized double-blind placebo-controlled clinical trial was performed among 60 pregnant women at risk for pre-eclampsia according to abnormal uterine artery Doppler waveform. Subjects were randomly divided into 2 groups to receive 50 000 IU vitamin D supplements (n=30) or receive placebo (n=30) every 2 weeks from 20 to 32 weeks of gestation. Fasting blood samples were taken at baseline study and 12 weeks after the intervention to quantify relevant variables. Newborn’s anthropometric measurements were determined. Pregnant women who received cholecalciferol supplements had significantly increased serum 25-hydroxyvitamin D concentrations (+17.92±2.28 vs. +0.27±3.19 ng/ml, p<0.001) compared with the placebo. The administration of cholecalciferol supplements, compared with the placebo, resulted in significant differences in serum insulin concentrations (+1.08±6.80 vs. +9.57±10.32 μIU/ml, p<0.001), homeostasis model of assessment-insulin resistance (HOMA-IR) (+0.19±1.47 vs. +2.10±2.67, p<0.001), homeostatic model assessment-beta cell function (HOMA-B) (+5.82±29.58 vs. +39.81±38.00, p<0.001) and quantitative insulin sensitivity check index (QUICKI) score (-0.009±0.03 vs. -0.04±0.03, p=0.004). Furthermore, cholecalciferol-supplemented pregnant women had increased HDL-cholesterol concentrations (+2.67 ± 8.83 vs. -3.23±7.76 mg/dl, p=0.008) compared with the placebo. Finally, cholecalciferol supplementation led to a significant rise in plasma total antioxidant capacity (TAC) concentrations (+79.00±136.69 vs. -66.91±176.02 mmol/l, p=0.001) compared with the placebo. Totally, the administration of cholecalciferol supplements among pregnant women at risk for pre-eclampsia for 12 weeks had favorable effects on insulin metabolism parameters, serum HDL-cholesterol, and plasma TAC concentrations.
Be well!
JP
March 30th, 2016 at 5:45 pm
Updated 03/30/16:
http://www.nature.com/ejcn/journal/vaop/ncurrent/abs/ejcn201651a.html
European Journal of Clinical Nutrition advance online publication 30 March 2016
Association of seasonal serum 25-hydroxyvitamin D levels with disability and relapses in relapsing-remitting multiple sclerosis
Background/Objectives: The aim of this study was to evaluate the association of serum 25-hydroxyvitamin D (25(OH)D) with disability and frequency of relapses in relapsing-remitting multiple sclerosis (MS) patients.
Subjects/Methods: The study included 184 patients with relapsing-remitting MS who were receiving immune-modulating drugs and no vitamin D supplementation. The concentration of 25(OH)D was measured in February and August 2014. The level of disability was assessed twice according to the Expanded Disability Status Scale (EDSS). The patients were divided into two groups: EDSS 0.0–2 and 2.5–4. The control group comprised 58 age- and sex-matched healthy subjects. The 25(OH)D levels were compared with the occurrence of relapses and the level of disability.
Results: Mean serum 25(OH)D concentrations were significantly lower in winter in both MS patients and controls. Winter level of 25(OH)D was significantly lower in severe MS cases (EDSS 2.5–4.0) than in mild cases (EDSS 0.0–2.0) (P=0.022), and in the controls (P=0.008), especially in females (r=0.38, P=0.0015). Logistic regression analysis showed the winter serum 25(OH)D was significantly associated with MS (odds ratio 0.925; 95% confidence interval, 0.822–0.970). Serum 25(OH)D levels were significantly lower in MS patients with relapses than in those without relapses both in winter, and in summer.
Conclusions: Hypovitaminosis D was more prevalent during winter than summer, both in the sample group and the control, especially in female MS patients with higher levels of disability. Low vitamin D levels are associated with a more severe course of disease and an increased number of relapses.
Be well!
JP
June 27th, 2018 at 11:51 pm
Updated 06/27/18:
http://jaha.ahajournals.org/content/7/13/e008814.long
J Am Heart Assoc. 2018 Jun 25;7(13).
Tea Consumption and Longitudinal Change in High-Density Lipoprotein Cholesterol Concentration in Chinese Adults.
BACKGROUND: The relation between tea consumption and age-related changes in high-density lipoprotein cholesterol (HDL-C) concentrations remains unclear, and longitudinal human data are limited. The aim of current study was to examine the relation between tea intake and longitudinal change in HDL-C concentrations.
METHODS AND RESULTS: Baseline (2006) tea consumption was assessed via a questionnaire, and plasma HDL-C concentrations were measured in 2006, 2008, 2010, and 2012 among 80 182 individuals (49±12 years of age) who did not have cardiovascular diseases or cancer, or did not use cholesterol-lowering agents both at baseline (2006) and during the follow-up period (2006-2012). The associations between baseline tea consumption and rate of change in HDL-C concentrations were examined using generalized estimating equation models. Tea consumption was inversely associated with a decreased rate of HDL-C concentrations (P-trend <0.0001) in the fully adjusted model. The adjusted mean difference in the HDL-C decreased rate was 0.010 (95% confidence interval, 0.008, 0.012) mmol/L per year for tea consumers versus nonconsumers (never or less than once/month group). Interactions between tea consumption and age, sex, lifestyle scores, and metabolic syndrome (all P-interaction <0.0001) were identified. The associations between greater tea consumption and slower decrease in HDL-C concentrations were more pronounced in men, individuals aged 60 or older, individuals with a lower lifestyle score, and individuals with metabolic syndrome (all P-trend <0.0001).
CONCLUSIONS: Tea consumption was associated with slower age-related decreases in HDL-C concentrations during 6 years of follow-up.
Be well!
JP