Addiction Alternatives
August 2, 2010 Written by JP [Font too small?]It’s hard to imagine any community that isn’t profoundly touched by addictive and/or compulsive disorders. The specific behaviors and substances involved vary but the end results are predictably ruinous, unless an effective intervention takes place. Alternative therapies are rarely used as primary treatment options for serious addictions which frequently lead to incarceration or permanent health consequences. However, a relatively new string of scientific studies do point to the utility of complementary approaches as an adjunct to conventional treatment. My Healthy Monday tip of the week is to consider mind-body techniques and natural remedies as part of a holistic treatment regime for addictions and compulsive behavior.

Regular readers of my site are familiar with my past which includes an eating disorder during my adolescence and a struggle with overweight in my adult life. My path to recovery involved a combination of psychotherapy in my youth and an informal Internet support group in recent years. Intensive psychotherapy and group counseling initially saved me from starvation at the hands of Anorexia Nervosa. The use of an online food diary and the backing of numerous low carb dieters provided the support I needed to lose over 85 lbs over the last few years. But the fact is, for many people, this type of “treatment” isn’t enough. More is needed.
While recently reviewing the medical literature, I identified several noteworthy forms of adjunctive therapies. Some will likely be more familiar to you and your physicians than others. The one thing they all have in common is at least some scientific evidence supporting their use in the field of addictive and compulsive conditions. Please note that just because I mention these options does not necessarily mean that they’re suitable for individual circumstances. Treating an addiction is a highly specialized process which requires the guidance of experts. The following data is simply intended to offer additional hope and resources.
Addiction Alternative #1 – N-Acetyl Cysteine (NAC)
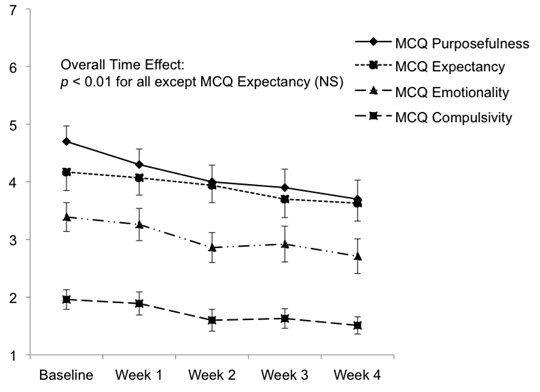
A current study presented in the American Journal of Addiction examined the effects of 2,400 mg/day of NAC in 24 cannabis dependent males and female with an average age of 18. This age group was targeted because marijuana use is significantly higher in adolescents (3.6%) and young adults (5.9%) as compared to older adults (.7%). Over the course of 4 weeks, the study participants were asked to take 1,200 mg of NAC twice-daily. During the period adverse reactions, “medication adherence” and marijuana use was documented. Marijuana use diaries indicated “a reduction in reported days per week of marijuana use over the course of NAC treatment“. In addition, several psychological components of cannabis dependence were also improved (compulsivity, emotionality and purposefulness) as assessed by a before-and-after Marijuana Craving Questionnaire. Side effects were relatively rare and mild in nature. (1)
In their concluding remarks, the authors of the pilot cannabis trial noted “prior NAC treatment studies in cocaine and nicotine dependent individuals”. They could have also mentioned that NAC has shown promising results in relation to other addictive and compulsive behaviors such as impulsive/obsessive hair pulling, nail biting and pathological gambling. (2,3,4,5,6)
Addiction Alternative #2 – Meditation and Mind-Body Therapies
The July 2010 edition of the Journal of Alternative and Complementary Medicine reports that Qigong meditation was better accepted and more effective than “Stress Management and Relaxation Training (SMART)” in a group of 248 men and women undergoing “residential addiction treatment”. Those practicing daily meditation noted a greater reduction in cravings and withdrawal symptoms than those using the SMART approach. Other forms of meditation including mindfulness meditation, Vipassana meditation and meditation + yoga have also resulted in improved treatment outcomes in various populations including substance abuse among prisoners. (7,8,9,10)
Another mind-body intervention referred to as “surfing the urge” recently made headlines in the medical journal Psychology of Addictive Behaviors. Over the course of one week, a group 123 undergraduate smokers applied this practice or not to their daily routine. Those who engaged in this “brief mindfulness-based therapy” smoked fewer cigarettes by apparently changing their response to urges to smoke. According to the National Institute of Alcohol Abuse and Alcoholism, “urge surfing” can best be described as a three-part process which involves:
- Taking inventory of how you experience cravings by allowing your attention to “wander through your body” and “notice where in your body you experience your cravings”.
- Focus on a single area where you experience your craving. Pay attention to the sensations you feel. Acknowledge and stay with the feeling. Don’t try to escape it.
- Repeat this sensory experience in all of the places where you physically feel the cravings.
The process isn’t intended to necessarily diminish cravings but rather allow one to experience them in a different way. One description summarizes it thusly, “Urges are a lot like ocean waves. They are small when they start, grow in size, and then break up and dissipate. You can imagine yourself as a surfer who will ride the wave, staying on top of it until it crests, breaks, and turns into less powerful, foamy surf”. (11,12,13)
Addiction Alternative #3 – Acetyl-L-Carnitine (ALC)
A new Italian study suggests that acetyl-l-carnitine (ALC) may diminish alcohol cravings and improve relapse prevention in alcohol dependent subjects. A randomized, double-blind, placebo controlled trial in 64 alcoholic patients revealed that 1,000 mg – 3,000 mg/day of ALC increased the likelihood of alcohol abstinence and lead to a decline in cravings for alcoholic beverages after just 10 days of treatment. These results were based on a 90 day preliminary evaluation. The conclusion states that, “ALC can reduce craving and the first time to drink” and that “ALC use was safe”. To the best of my knowledge, this is first human trial involving ALC in addiction treatment. Two animal studies from 2004 and 2006 were probably the basis for the above human study. Those initial experiments hinted at the potential of ALC in rats that were dependent on cocaine and methamphetamine. (14,15,16)
Addiction Alternative #4 – Rhodiola Rosea
Rhodiola rosea has traditionally been used as an adaptogen to assist the body and mind adapt to mental and physical stressors. Emerging evidence in animal models offers hope that this adaptogenic activity may one day support humans who are addicted to drugs. The most current example can be found in the February 2010 issue of the Journal of Psychopharmacology. It describes an experiment in which Rhodiola rosea extract “significantly and dose-dependently attenuated both development and expression of morphine dependence after chronic and acute administration. These data suggest the Rhodiola rosea may have human therapeutic potential for treatment of opioid addiction”. Two additional investigations support this contention by showing that Rhoidola extracts aid with nicotine cessation and withdrawal and may attenuate substance seeking behavior. (17,18,19)
In terms of the quality of evidence, NAC and the mind-body approaches I’ve mentioned are leading the pack for realistic alternatives in addiction treatment. But ALC and Rhodiola rosea are therapeutic candidates that merit monitoring and consideration if additional research continues to show promise. At present, new studies are planned or are underway that may help researchers better understand whether natural remedies offer true hope to those living with addictive and compulsive disorders. I’ll be sure to keep a close eye out for those results and relay the information to you in future columns. (20,21,22,23,24)
Note: Please check out the “Comments & Updates” section of this blog – at the bottom of the page. You can find the latest research about this topic there!
Be well!
JP
Tags: Addiction, Meditation, NAC
Posted in Alternative Therapies, Mental Health, Nutritional Supplements

August 3rd, 2010 at 7:49 pm
I am a recovering alcoholic, gambler, and other addiction problems. I published a book, Gripped by Gambling, where the readers can follow the destructive path of the compulsive gambler, a prison sentence, and then on to the recovery road. I am currently publishing a second book, Switching Addictions, that describes the challenges the addict encounters as they work toward recovery. I also publish an online newsletter, Women Helping Women, which has been on-line for more than ten years and is read by women around the world. I would like to suggest you add the link to the newsletter to your link page.
Sincerely,
Marilyn Lancelot
September 27th, 2013 at 4:36 pm
Your web page is very informative and helpful to discussions such as addictions.
Thank you for sharing your page.
All the page,
Sharon
April 13th, 2015 at 2:31 pm
Update: 4/13/15:
http://ntr.oxfordjournals.org/content/early/2015/04/11/ntr.ntv074.abstract
Nicotine Tob Res. 2015 Apr 11.
Effect of Brief Mindfulness Practice on Self-Reported Affect, Craving, and Smoking: A Pilot Randomized Controlled Trial Using Ecological Momentary Assessment.
INTRODUCTION: Despite efficacious pharmacological and behavioral treatments, most smokers attempt to quit without assistance and fail to quit. Mindfulness practice may be useful in smoking cessation.
METHODS: This ecological momentary assessment (EMA) study was a pilot parallel group randomized controlled trial of a brief mindfulness practice (Brief-MP) intervention on self-reported smoking behavior delivered to smokers on a Personal Digital Assistant (PDA) in the field. Adult community smokers (N = 44) were randomly assigned to a Brief-MP (n = 24) or Control (sham meditation; n = 20) group. Participants were instructed to smoke as much or as little as they liked. Participants carried a PDA for two weeks and were instructed to initiate 20 minutes of meditation (or control) training on the PDA daily, completing an assessment of cognitive and affective processes immediately afterwards. Additionally, they completed assessments at random times up to four times per day. Primary outcome variables were negative affect, craving, and cigarettes smoked per day, all self-reported.
RESULTS: Thirty-seven participants provided EMA data totaling 1874 assessments. Linear Mixed Model analyses on EMA data revealed that Brief-MP (vs. Control) reduced overall negative affect, F [1, 1798] = 13.8, p = .0002; reduced craving immediately post-meditation, (Group x Assessment Type interaction, F [2, 1796] = 12.3, p = .0001); and reduced cigarettes smoked per day over time (Group x Day interaction, F [1, 436] = 5.50, p = .01).
CONCLUSIONS: Brief-MP administered in the field reduced negative affect, craving, and cigarette use, suggesting it may be a useful treatment.
Be well!
JP
June 8th, 2015 at 5:41 pm
Update 06/08/15:
http://www.drugandalcoholdependence.com/article/S0376-8716%2815%2900261-6/abstract
Drug Alcohol Depend. 2015 May 27.
A single dose of kudzu extract reduces alcohol consumption in a binge drinking paradigm.
BACKGROUND: Overconsumption of alcohol has significant negative effects on an individual’s health and contributes to an enormous economic impact on society as a whole. Pharmacotherapies to curb excessive drinking are important for treating alcohol use disorders.
METHODS: Twenty (20) men participated in a placebo-controlled, double-blind, between subjects design experiment (n=10/group) that tested the effects of kudzu extract (Alkontrol-Herbal™) for its ability to alter alcohol consumption in a natural settings laboratory. A single dose of kudzu extract (2g total with an active isoflavone content of 520mg) or placebo was administered 2.5h before the onset of a 90min afternoon drinking session during which participants had the opportunity to drink up to 6 beers ad libitum; water and juice were always available as alternative beverages.
RESULTS: During the baseline session, the placebo-randomized group consumed 2.7±0.78 beers before treatment and increased consumption to 3.4±1.1 beers after treatment. The kudzu group significantly reduced consumption from 3.0±1.7 at baseline to 1.9±1.3 beers after treatment. The placebo-treated group opened 33 beers during baseline conditions and 38 following treatment whereas the kudzu-treated group opened 32 beers during baseline conditions and only 21 following treatment. Additionally, kudzu-treated participants drank slower.
CONCLUSION: This is the first demonstration that a single dose of kudzu extract quickly reduces alcohol consumption in a binge drinking paradigm. These data add to the mounting clinical evidence that kudzu extract may be a safe and effective adjunctive pharmacotherapy for alcohol abuse and dependence.
Be well!
JP
July 15th, 2015 at 9:30 pm
Updated 07/15/15:
http://www.ncbi.nlm.nih.gov/pubmed/26170596
Int J Yoga. 2015 Jul-Dec;8(2):144-7.
Effectiveness of yogic breathing intervention on quality of life of opioid dependent users.
INTRODUCTION: The quality of life (QOL) of substance users is known to be impaired. Sudarshan Kriya Yoga (SKY), a yogic breathing program has potential to improve QOL and needs evaluation in an Indian setting.
AIMS: Study aimed to assess changes in QOL in treatment seeking male opioid dependent users following practice of SKY program.
SETTINGS AND DESIGN: Users were randomized into study (n = 55) and control group (n = 29). Study group besides standard treatment (long term pharmacotherapy with buprenorphine in flexible dosing schedule) underwent a 3 days, 12 h SKY program while control group received standard treatment alone.
MATERIALS AND METHODS: World Health Organization QOL-brief scale was used to measure QOL and urine tested to assess recent drug use. Assessments were made at baseline and at 3 and 6 months.
STATISTICAL ANALYSIS: Data were analyzed using generalized estimation equation to assess within group change with time and the overall difference between groups for changes at assessment points.
RESULTS: Overtime within study group, all four QOL domain scores were significantly higher at 6 months. Between group comparison showed significant increase in physical (P < 0.05); psychological (P < 0.001) and environment domains (P < 0.001) for study group while control group showed significant changes in social relationship domain only. Urine screening results were negative for study group indicating no drug use at 6 months. CONCLUSION: SKY as a complementary therapy was found beneficial in improving QOL for group practicing it and is recommended for use as low cost and low-risk adjunct in substance treatment settings in India. Be well! JP
July 20th, 2015 at 7:58 pm
Updated 07/20/15:
http://www.sciencedirect.com/science/article/pii/S0195666315003323
Appetite. 2015 Jul 15. pii: S0195-6663(15)00332-3.
Effectiveness of lifestyle interventions to reduce binge eating symptoms in African American and Hispanic women.
OBJECTIVE: Lifestyle interventions that promote physical activity and healthy dietary habits may reduce binge eating symptoms and be more feasible and sustainable among ethnic minority women, who are less likely to seek clinical treatment for eating disorders. The purpose of this study was to investigate (1) whether participating in a lifestyle intervention is a feasible way to decrease binge eating symptoms (BES) and (2) whether changes in BES differed by intervention (physical activity vs. dietary habits) and binge eating status at baseline (binger eater vs. non-binge eater) in African American and Hispanic women.
METHOD: Health Is Power (HIP) was a longitudinal randomized controlled trial to promote physical activity and improve dietary habits. Women (N=180) who completed anthropometric measures and questionnaires assessing fruit and vegetable and dietary fat intake, BES and demographics at baseline and post-intervention six months later were included in the current study.
RESULTS: Over one-fourth (27.8%) of participants were categorized as binge-eaters. Repeated measures ANOVA demonstrated significant two- and three-way interactions. Decreases in BES over time were greater in binge eaters than in non-binge eaters (F(1,164)=33.253, p<.001), and women classified as binge eaters who participated in the physical activity intervention reported greater decreases in BES than non-binge eaters in the dietary habits intervention (F(1,157)=5.170, p=.024). DISCUSSION: Findings suggest behavioral interventions to increase physical activity may lead to reductions in BES among ethnic minority women and ultimately reduce the prevalence of binge eating disorder and health disparities in this population. Be well! JP
October 8th, 2015 at 10:51 am
Works to reduce cannabis cravings.
30 year user reports no cravings with one week of Rhodiola rosea intake.
October 8th, 2015 at 11:22 am
Thanks for relaying that, Sam. Good news!
If you’re willing, I’d like to hear more about it. For instance, what Rhodiola product was used? Dosage? How long did it take for the cravings to diminish?
Be well!
JP
March 31st, 2016 at 2:38 pm
Updated 03/31/16:
http://www.sciencedirect.com/science/article/pii/S0944711316000519
Phytomedicine. 2016 Feb 24.
Rhodiola rosea L. as a putative botanical antidepressant.
Rhodiola rosea (R. rosea) is a botanical adaptogen with putative anti-stress and antidepressant properties. Evidence-based data supporting the effectiveness of R. rosea for depression in adults is limited, and therefore a comprehensive review of available animal and human studies suggesting a putative antidepressant action is warranted.
PURPOSE: A review of the literature was undertaken to ascertain studies of possible antidepressant mechanisms of action and studies of the safety and effectiveness of R. rosea extracts in animals and adult humans.
METHODS: A search of MEDLINE and the Russian state library database was conducted (up to October 2015) on R. rosea.
RESULTS: Mechanism of action: R. rosea extracts and its purified constituent, salidroside, has been shown to produce a variety of mediator interactions with several molecular networks of neuroendocrine-immune and neurotransmitter receptor systems likely to be involved in the pathophysiology of depression. A wide variety of preclinical in vivo and ex vivo studies with laboratory animals suggests the presence of several biochemical and pharmacological antidepressant-like actions.
EFFECTIVENESS: Clinical assessment of R. rosea L. rhizome extracts in humans with various depressive syndromes is based upon results from two randomized, double-blind, placebo-controlled trials of 146 subjects with major depressive disorder and seven open-label studies totaling 714 individuals with stress-induced mild depression (diagnosed as asthenic syndrome or psychoneurosis). Overall, results of these studies suggests a possible antidepressant action for R. rosea extract in adult humans.
SAFETY: In contrast to most conventional antidepressants, R. rosea extract appears to be well-tolerated in short-term studies with a favorable safety profile.
CONCLUSIONS: R. rosea demonstrates multi-target effects on various levels of the regulation of cell response to stress, affecting various components of the neuroendocrine, neurotransmitter receptor and molecular networks associated with possible beneficial effects on mood.
Be well!
JP
April 19th, 2016 at 12:06 pm
Updated 04/19/16:
http://www.ncbi.nlm.nih.gov/pubmed/27089525
Altern Ther Health Med. 2016 Apr;22(S1):8-13.
Pilot Study on the Homeopathic Treatment of Binge Eating in Males.
Context • Frequent binge eating is often a symptom of an underlying eating disorder, such as bulimia nervosa (BN) or binge eating disorder (BED). The role of homeopathy in the treatment of binge eating remains poorly explored.
Objective • The study intended to measure the efficacy of individualized homeopathic treatment for binge eating in adult males.
Design • This case study was a 9-wk pilot using an embedded, mixed-methods design. A 3-wk baseline period was followed by a 6-wk treatment period.
Setting • The setting was the Homeopathic Health Clinic at the University of Johannesburg in Johannesburg, South Africa.
Participants • Through purposive sampling, the research team recruited 15 Caucasian, male participants, aged 18-45 y, who were exhibiting binge eating.
Intervention • Individualized homeopathic remedies were prescribed to each participant.
Primary Outcome Measures • Participants were assessed by means of (1) a self-assessment calendar (SAC), recording the frequency and intensity of binging; (2) the Binge Eating Scale (BES), a psychometric evaluation of severity; and (3) case analysis evaluating changes with time.
Results • Ten participants completed the study. The study found a statistically significant improvement with regard to the BES (P = .003) and the SAC (P = .006), with a large effect size, indicating that a decrease occurred in the severity and frequency of binging behavior during the study period.
Conclusions • This small study showed the potential benefits of individualized homeopathic treatment of binge eating in males, decreasing both the frequency and severity of binging episodes. Follow-up studies are recommended to explore this treatment modality as a complementary therapeutic option in eating disorders characterized by binge eating.
Be well!
JP
May 26th, 2016 at 12:47 pm
Updated 05/25/16
http://www.tandfonline.com/doi/abs/10.3109/00952990.2016.1153646?journalCode=iada20
Am J Drug Alcohol Abuse. 2016 May 21:1-10.
Beneficial effects of Tai Chi for amphetamine-type stimulant dependence: a pilot study.
BACKGROUND: Tai Chi is a traditional Chinese sport that is classified as a moderate exercise. Recent studies have evaluated the effectiveness of Tai Chi in substance abuse rehabilitation.
OBJECTIVES: The aim of this study was to assess the quality of life and physical effects of a Tai Chi intervention on individuals with amphetamine-type stimulant (stimulant) dependence.
METHODS: Sixty male subjects with stimulant dependence from a Shanghai Mandatory Detoxification and Rehabilitation Center participated in a 12-week trial. Tai Chi was used as an intervention in the experimental group (n = 30). The control group (n = 29) underwent standard care, which included recreation activity, gesture language exercise, and self-education. Outcome measures included the quality of life for drug addiction (QOL-DA) questionnaire [four scales consisting of physiology (e.g., energy level), psychology (e.g., depression), symptoms (e.g., physical symptoms), society (e.g., interpersonal) and fitness evaluations (assessed by body mass index, body fat, hand-grip, flexibility, balance)]. Repeated measures were used to analyze the changes over time.
RESULTS: Test scores of the QOL-DA in the Tai Chi group significantly increased after 12 weeks in the following areas: physiology, 8.71 (p = 0.005), symptoms, 4.34 (p = 0.042), society, 15.79 (p < 0.001), and total score, 10.60 (p = 0.002). A post hoc test further revealed that quality of life improved in the Tai Chi group but not in the standard care group. Physical results showed a significant interaction with balance(F(1,56) = 6.92, p = 0.011); participants in the Tai Chi group improved by 10 s while there was no change in the standard care group. Although there were no significant interactions in the fitness outcomes (i.e., hand-grip and sit-and-reach tests), the within-group factor displayed significant changes in body fat (F(1,56) = 27.79, p < 0.001) in both groups.
CONCLUSION: This study demonstrates that Tai Chi is a promising exercise that improves quality of life for individuals with stimulant dependence.
Be well!
JP
July 18th, 2016 at 11:11 pm
Updated 07/18/16:
http://www.contemporaryclinicaltrials.com/article/S1551-7144(16)30094-5/abstract
Contemp Clin Trials. 2016 Jun 29;49:126-133.
Randomized controlled trial of a 12-month computerized mindfulness-based intervention for obese patients with binge eating disorder: The MindOb study protocol.
BACKGROUND: Mindfulness-based interventions for healthy behaviors such as exercise and dietary modifications have aroused growing interest. This study aims to test the effectiveness of a mindfulness-based intervention for the reduction of impulsive eating and the improvement of motivation to exercise among obese individuals.
METHODS: One-hundred and twenty obese outpatients, aged 18 to 65years, diagnosed with a binge eating disorder, will be randomly assigned to one of the three following groups: mindfulness practice, sham meditation, or treatment as usual control. The tested intervention consists of a 1-year computerized mindfulness-based program. Mindfulness sessions are audio recordings that the patients are asked to listen to, 10min every day. Self-reported questionnaires measuring impulsive eating, motivation to exercise, physical activity level, mood, and mindfulness skills are filled in at baseline, 1, 6, and 12months. Physical activity, calories consumption, and biomarkers are measured with more objective measurement tools at baseline, 6months and 12months.
CONCLUSION: Mindfulness, as both a de-automation element and as a moderator of motivation to exercise, can lead to the reduction of impulsive eating and also to an increase in levels of physical activity. These effects could cause weight loss in obese patients suffering from binge eating disorder.
Be well!
JP
August 16th, 2016 at 12:07 pm
Updated 08/16/16:
http://www.ncbi.nlm.nih.gov/pubmed/27521979
Addict Behav. 2016 Aug 4;63:172-177.
Alcohol use during a trial of N-acetylcysteine for adolescent marijuana cessation.
AIMS: Current adolescent alcohol treatments have modest effects and high relapse rates. Evaluation of novel pharmacotherapy treatment is warranted. N-acetylcysteine (NAC), an over-the-counter antioxidant supplement with glutamatergic properties, is a promising treatment for marijuana cessation in adolescents; however, its effects on adolescent drinking have not been examined. To that end, this secondary analysis evaluated: (1) the effect of NAC vs. placebo on alcohol use over an eight-week adolescent marijuana cessation trial and (2) the role of marijuana cessation and reduction on subsequent alcohol use.
METHODS: Marijuana-dependent adolescents (ages 15-21; N=116) interested in treatment were randomized to NAC 1200mg or matched placebo twice daily for eightweeks. Participants were not required to be alcohol users or interested in alcohol cessation to qualify.
RESULTS: There were no demographic or baseline alcohol use differences between participants randomized to NAC vs. placebo (ps>0.05). Of the 89 participants returning for ≥one visit following randomization, 77 reported ≥one alcoholic drink in the 30days prior to study entry and averaged 1.3 (SD=1.4) binge drinking days per week. During treatment, less marijuana use (measured via urine cannabinoid levels) was associated with less alcohol use in the NAC-treated group but not in the placebo-treated group (p=0.016).
CONCLUSIONS: There was no evidence of compensatory alcohol use during marijuana treatment. In fact, in the NAC group, lower levels of marijuana use were associated with less alcohol use, suggesting NAC effects may generalize to other substances and could be useful in decreasing adolescent alcohol use. NAC trials specifically focused on alcohol-using adolescents are warranted.
Be well!
JP
November 2nd, 2016 at 1:15 pm
Updated 11/02/16:
http://www.psychiatrist.com/JCP/article/Pages/2016/aheadofprint/15m10239.aspx
J Clin Psychiatry. 2016 Oct 11.
A Double-Blind, Randomized, Controlled Pilot Trial of N-Acetylcysteine in Veterans With Posttraumatic Stress Disorder and Substance Use Disorders.
OBJECTIVE: The antioxidant N-acetylcysteine is being increasingly investigated as a therapeutic agent in the treatment of substance use disorders (SUDs). This study explored the efficacy of N-acetylcysteine in the treatment of posttraumatic stress disorder (PTSD), which frequently co-occurs with SUD and shares impaired prefrontal cortex regulation of basal ganglia circuitry, in particular at glutamate synapses in the nucleus accumbens.
METHODS: Veterans with PTSD and SUD per DSM-IV criteria (N = 35) were randomly assigned to receive a double-blind, 8-week course of N-acetylcysteine (2,400 mg/d) or placebo plus cognitive-behavioral therapy for SUD (between March 2013 and April 2014). Primary outcome measures included PTSD symptoms (Clinician-Administered PTSD Scale, PTSD Checklist-Military) and craving (Visual Analog Scale). Substance use and depression were also assessed.
RESULTS: Participants treated with N-acetylcysteine compared to placebo evidenced significant improvements in PTSD symptoms, craving, and depression (β values < -0.33; P values < .05). Substance use was low for both groups, and no significant between-group differences were observed. N-acetylcysteine was well tolerated, and retention was high. CONCLUSIONS: This is the first randomized controlled trial to investigate N-acetylcysteine as a pharmacologic treatment for PTSD and SUD. Although preliminary, the findings provide initial support for the use of N-acetylcysteine in combination with psychotherapy among individuals with co-occurring PTSD and SUD. Be well! JP
November 15th, 2016 at 11:58 pm
Updated 11/15/16:
http://online.liebertpub.com/doi/10.1089/acm.2016.0246
J Altern Complement Med. 2016 Nov 9.
Effects of T’ai Chi on Serotonin, Nicotine Dependency, Depression, and Anger in Hospitalized Alcohol-Dependent Patients.
OBJECTIVES: The aim of this study was to investigate the effects of t’ai chi on blood serotonin levels, nicotine dependence, depression, and anger in hospitalized alcohol-dependent patients.
METHOD: This study followed an experimental and nonequivalent control group in a non-synchronized design. It was performed in a hospital located in Young Ju city, Korea, from April to August 2013. Thirty-eight patients who were hospitalized with alcohol dependence were included. They were randomly divided into an experimental and a control group, with 19 patients in each group. Patients in the experimental group practiced the 24-posture yang style t’ai chi for 50 min three times per week for 8 weeks as part of the routine hospital rehabilitation program, and those in the control group followed only the routine hospital rehabilitation program. The effect of treatment was measured using blood serotonin levels and a questionnaire on nicotine dependence, depression, and anger. Both measurements were performed before and after 8 weeks of intervention. Data were analyzed using the t-test, chi-square test, and paired t-tests.
RESULTS: The experimental group showed a significantly increased blood serotonin level (p = 0.001) and significantly reduced nicotine dependence, depression, and anger (p = 0.001) than the control group did after 8 weeks of treatment.
CONCLUSIONS: T’ai chi was shown to be an effective nursing intervention in hospitalized alcohol-dependent patients.
Be well!
JP
June 24th, 2017 at 6:42 pm
Updated 06/24/17:
https://www.ncbi.nlm.nih.gov/pubmed/28642082
Prog Neuropsychopharmacol Biol Psychiatry. 2017 Jun 19.
Clinical trial of the effects of vitamin D supplementation on psychological symptoms and metabolic profiles in maintenance methadone treatment patients.
BACKGROUND: Vitamin D deficiency may be associated with some complications including nonspecific musculoskeletal pain and periodontal disease in maintenance methadone treatment (MMT) patients. This study was designed to determine the effect of vitamin D supplementation on psychological symptoms and metabolic profiles in MMT patients.
METHODS: This randomized, double-blind, placebo-controlled, clinical trial was carried out among 68 MMT patients. Participants were randomly allocated to receive either 50,000IU vitamin D supplements (n=34) or placebo (n=34) every 2weeks for 12weeks. Fasting blood samples were taken at baseline and post-intervention to evaluate relevant variables.
RESULTS: After the 12-week intervention, serum 25(OH) vitamin D levels significantly increased in the intervention group compared with the placebo group (+8.1±4.9 vs. -0.4±3.0, P<0.001). In addition, vitamin D supplementation significantly improved Pittsburgh Sleep Quality Index (-1.5±2.2 vs. -0.2±2.3, P=0.02) and Beck Depression Inventory (-4.8±7.3 vs. -1.5±6.1, P=0.04) compared with the placebo. Patients who received vitamin D supplements had significantly decreased fasting plasma glucose (-7.5±10.6 vs. +0.3±10.7mg/dL, P=0.004), serum insulin levels (-3.6±5.3 vs. -0.9±3.5 μIU/mL, P=0.01), homeostasis model of assessment-insulin resistance (-1.0±1.3 vs. -0.2±0.7, P=0.003), serum triglycerides (-9.6±30.8 vs. +15.6±30.2mg/dL, P=0.001), total- (-8.7±20.9 vs. +11.0±27.4mg/dL, P=0.001) and LDL-cholesterol (-11.1±17.9 vs. +5.9±27.5mg/dL, P=0.004) compared with the placebo. Additionally, vitamin D intake resulted in a significant decrease in serum high sensitivity C-reactive protein (-2.2±4.2 vs. +2.0±3.7mg/L, P<0.001), and significant increases plasma total antioxidant capacity (+26.2±99.8 vs. -86.3±127.5mmol/L, P<0.001) and glutathione levels (+292.3±172.4 vs. +48.9±208.9μmol/L, P<0.001) compared with the placebo. There was no significant effect of vitamin D supplementation on serum HDL-cholesterol, and other markers of insulin metabolism, inflammation and oxidative stress.
CONCLUSIONS: Totally, taking 50,000IU vitamin D supplement every 2weeks for 12weeks in MMT patients had beneficial effects on psychological symptoms and few metabolic profiles.
Be well!
JP
September 30th, 2017 at 3:52 pm
Updated 09/30/17:
https://www.ncbi.nlm.nih.gov/pubmed/28960384
Int J Eat Disord. 2017 Sep 27.
Randomized controlled trial comparing smartphone assisted versus traditional guided self-help for adults with binge eating.
OBJECTIVE: Guided self-help treatments based on cognitive-behavior therapy (CBT-GSH) are efficacious for binge eating. With limited availability of CBT-GSH in the community, mobile technology offers a means to increase use of these interventions. The purpose of this study was to test the initial efficacy of Noom Monitor, a smartphone application designed to facilitate CBT-GSH (CBT-GSH + Noom), on study retention, adherence, and eating disorder symptoms compared to traditional CBT-GSH.
METHOD: Sixty-six men and women with DSM-5 binge-eating disorder (BED) or bulimia nervosa (BN) were randomized to receive eight sessions of CBT-GSH + Noom (n = 33) or CBT-GSH (n = 33) over 12 weeks. Primary symptom outcomes were eating disorder examination objective bulimic episodes (OBEs), subjective bulimic episodes (SBEs), and compensatory behaviors. Assessments were collected at 0, 4, 8, 12, 24, and 36 weeks. Behavioral outcomes were modeled using zero-inflated negative-binomial latent growth curve models with intent-to-treat.
RESULTS: There was a significant effect of treatment on change in OBEs (β = -0.84, 95% CI = -1.49, -0.19) favoring CBT-GSH + Noom. Remission rates were not statistically different between treatments for OBEs (βlogit = -0.73, 95% CI = -1.86, 3.27; CBT-GSH-Noom = 17/27, 63.0% vs. CBT-GSH 11/27, 40.7%, NNT = 4.5), but CBT-GSH-Noom participants reported greater meal and snack adherence and regular meal adherence mediated treatment effects on OBEs. The treatments did not differ at the 6-month follow-up.
DISCUSSION: Smartphone applications for the treatment binge eating appear to have advantages for adherence, a critical component of treatment dissemination.
Be well!
JP
January 25th, 2018 at 12:04 am
Updated 1/24/18:
https://www.hindawi.com/journals/amed/2017/1079132/
Adv Med. 2017;2017:1079132.
The Impact of Saffron on Symptoms of Withdrawal Syndrome in Patients Undergoing Maintenance Treatment for Opioid Addiction in Sabzevar Parish in 2017.
Background and Objective: Drug dependence is one of the serious problems around the world. Saffron is one of those beneficial medicinal plants which is embedded with a similar mechanism to methadone (e.g., inhibition of serotonin reuptake). Thus, it can be helpful in reducing the withdrawal symptoms. The aim of this study was to reduce the daily dose of methadone usage and reduce its side effects using saffron in the form of medicinal supplements.
Methodology: This study was categorized as a clinical trial. Accordingly, 44 clients of addiction treatment centers in Sabzevar parish were randomly selected to participate in this study in 2016-2017. While the experimental group was treated with methadone syrup and self-made saffron capsules, the control group received methadone syrup and placebo capsules.
Results: The results showed that the use of saffron and methadone alleviated the symptoms of withdrawal syndrome (p<0.001).
Conclusion: Having reviewed the research participants, it was indicated that the introduction of saffron alleviated the symptoms of withdrawal syndrome in patients undergoing maintenance treatment for opioid addiction. Thus, it seems rational to make use of saffron in combination with methadone in order to alleviate the symptoms of withdrawal syndrome.
Be well!
JP
March 3rd, 2018 at 5:20 pm
Updated 03/03/18:
http://www.journalofsubstanceabusetreatment.com/article/S0740-5472(17)30436-1/abstract
J Subst Abuse Treat. 2018 Apr;87:23-30.
Integration of Transcendental Meditation® (TM) into alcohol use disorder (AUD) treatment.
AIMS: Maladaptive responses to stress are thought to play a role in addiction and relapse. Transcendental Meditation (TM) is a popular meditation technique with promising clinical applications. This study sought to: (a) examine the feasibility of providing TM during AUD treatment; (b) compare outcomes for TM vs. treatment as usual (TAU); and (c) investigate the relationship between TM practice and outcomes.
METHODS: Meditation-naïve adults with primary AUD (N = 60; 35% female, 60% white) newly admitted to inpatient treatment were recruited in sequential cohorts (30 receiving TAU and 30 receiving TM training). Assessments were conducted at baseline and 3-months post-discharge.
RESULTS: Integrating TM into inpatient AUD treatment was feasible. Uptake of TM was high (85% meditating on most of the past 30 days at follow-up; 61% closely adherent to recommended practice of twice-daily TM). Participants reported high satisfaction with TM. The sample as a whole improved on multiple measures after AUD treatment, but there were no significant differences between TM and TAU cohorts. However, those practicing TM twice-daily as recommended were less likely than the rest of the sample to return to any drinking (25% vs. 59%; p = .02) or heavy drinking post-discharge (0% vs. 47%, p < .001). Greater regularity of TM practice was inversely correlated with stress, psychological distress, craving, and alcohol use at follow-up. CONCLUSIONS: This study established the feasibility and acceptability of using TM during AUD treatment. Consistently practicing TM (but not just learning it) was associated with better outcomes. Be well! JP
September 5th, 2018 at 9:51 pm
Updated 09/05/18:
https://www.ncbi.nlm.nih.gov/pubmed/30177899
Front Psychol. 2018 Aug 20;9:1476.
Long-Term Effects of Tai Chi Intervention on Sleep and Mental Health of Female Individuals With Dependence on Amphetamine-Type Stimulants.
Previous studies provide evidence that Tai Chi (TC) can reduce the symptoms of sleep problems and be of benefit for the rehabilitation of substance abusers. In this study, we investigated if TC practice can improve sleep quality and mood of females who are dependent on amphetamine-type stimulant (ATS). Eighty subjects were randomly assigned to TC intervention and standard care (SC) for 6 months. We applied analysis of variance on repeated-measure with the year of drug dependence as the covariate to test the changes of the self-rated Pittsburg Sleep Quality Index (PSQI), Self-Rating Depression Scale (SDS), as well as fitness after 3 and 6 months. Relapse investigation was conducted by checking the database of China’s National Surveillance System on Drug Abuse and that of the Shanghai Drug Control Committee’s illicit drug dependents. Our investigation focused on the relapse of participants who had undergone and completed treatment in the Shanghai Mandatory Detoxification and Rehabilitation Center in 2015. The result showed that the PSQI scores of sleep duration [F(2, 92) = 9.86], need for sleep medications [F(2, 92) = 36.44] and daytime dysfunction [F(2, 92) = 5.15] were found to have a significant difference by time × group interaction after 6 months. SDS showed no significant difference between the two groups; however, the score of SDS in TC decreased after 6-month intervention, and no changes were observed in SC. Pulse rate had significantly decreased in the TC group compared with the SC group after 6 months. 9.5% (4) ATS dependents in TC and 26.3% (10) ATS dependents in SC were found to have relapsed. Our result suggested that TC had positive effects on sleep quality, depression and fitness. Long-term study demonstrated that TC may be a cheap and potential supplementary treatment for ATS-dependent individuals. TC may also be considered as an alternative exercise to escalate abstinence for ATS-dependent females.
Be well!
JP
November 26th, 2018 at 2:40 pm
Updated 11/26/18:
https://www.journalofsubstanceabusetreatment.com/article/S0740-5472(18)30243-5/abstract
J Subst Abuse Treat. 2019 Jan;96:58-64.
Raja yoga meditation and medication-assisted treatment for relapse prevention: A pilot study.
The continued need for advancement in evidence-based SUD treatment, as well as increases in treatment expense and decline in support from insurance providers, suggest that brief, innovative, and affordable treatments are needed. Meditation, spirituality, and adherence to medication-assisted treatments have all been shown to support abstinence. The current trial assessed effects of spiritually-based meditation, versus relaxation or standard treatment, on substance abstinence and psychological distress and dysfunction in a partially buprenorphine-supported (41.5%) treatment sample. Participants (N = 40) were recruited from an intensive outpatient treatment program, in which three treatment locations acted as separate experimental conditions. Abstinence was measured through urinalyses at baseline and weekly thereafter for the duration of the intervention. Psychological distress and dysfunction were assessed with a Likert-scaled questionnaire measuring symptoms typically associated with SUD. Co-varying for buprenorphine use, participants in the Meditation condition had better odds of remaining abstinent than participants in the Treatment-as-Usual (TAU) and Relaxation conditions. There were no significant differences in substance abstinence between the Relaxation and TAU conditions. Further, co-varying out baseline there were no significant differences at post-course in psychological distress and dysfunction between the three conditions. Results from this pilot trial suggest that this spiritually-informed approach may offer additive support to individuals in SUD treatment, as an aid to the meditative aspect of the 12 steps, or a non-12-step alternative spiritual supplement to standard SUD treatment.
Be well!
JP
February 18th, 2019 at 4:23 pm
Updated 02/18/19:
https://www.sciencedirect.com/science/article/pii/S0028390818305513?via%3Dihub
Neuropharmacology. 2019 Feb 4;149:27-34.
A ketogenic diet diminishes behavioral responses to cocaine in young adult male and female rats.
Ketogenic diets (KDs) are high fat, low carbohydrate formulations traditionally used to treat epilepsy; more recently, KDs have shown promise for a wide range of other neurological disorders. Drug addiction studies suggest that repeated exposure to drugs of abuse, including cocaine, results in a suite of neurobiological changes that includes neuroinflammation, decreased glucose metabolism, and disordered neurotransmission. Given that KDs positively regulate these factors, we addressed whether administration of a KD has potential as a novel therapy for drug addiction. In this study, male and female Sprague-Dawley rats were placed on a KD or a control diet (CD), beginning at five weeks of age and continuing through the end of behavioral testing. Three weeks after initiation of dietary treatments, rats received daily i.p. injections of cocaine (15 mg/kg) or saline vehicle for one week, were drug free for a subsequent week, and then all animals received a final challenge injection of 15 mg/kg cocaine. In the absence of cocaine injections, stereotyped locomotor responses were minimal and were unaffected by dietary treatment. In contrast, both males and females fed a KD exhibited decreased cocaine-induced stereotyped responses as compared to CD-fed rats. The sensitization of ambulatory responses was also disrupted in KD-fed rats. These results suggest that KDs directly impact dopamine-mediated behaviors, and hence may hold potential as a therapy for drug addiction.
Be well!
JP