Vitamin D and Lung Health
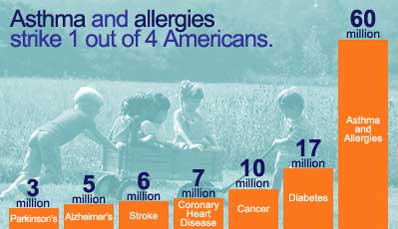
May 26, 2009 Written by JP [Font too small?]In the field of nutritional science, there is no hotter nutrient than Vitamin D. Scientists are steadfastly studying the effects of D on everything from arthritis to cardiovascular disease and even psychiatric conditions such as schizophrenia. One area of particular interest is that of Vitamin D deficiency and pulmonary health. There is a desperate need to identify preventive measures and safe treatments for lung conditions because of the shockingly large number of people who are affected by them. It is estimated that approximately 300 million people worldwide suffer from asthma alone, and that number is growing at a staggering pace.
Research presented on Wednesday at the American Thoracic Society’s 105th International Conference revealed a novel mechanism by which Vitamin D may help to slow or even halt the progression of asthma and COPD (Chronic Obstructive Pulmonary Disease). Scientists from the University of Pennsylvania described the ability of calcitriol (a form of Vitamin D) to reduce the growth of “airway smooth muscle” that is a hallmark of the progressive decline found in those with COPD and asthma. This type of “airway remodeling” brings about decreased lung function over time. (1)
In the current laboratory experiment, calcitriol and a powerful corticosteroid were both tested on lung cells provided by 12 asthmatic and healthy volunteers. Both substances are known to possess anti-inflammatory properties.
The researchers were surprised to find that the corticosteroid, commonly used to treat asthma, didn’t have much of an impact on the undesirable proliferation of the lung cells. On the other hand, Vitamin D showed a “dose-dependent” effect on the expansion of “airway smooth muscle”. These findings were so impressive that a human study in patients with severe asthma is already underway. It is expected to be completed in about a year.
There is also hope that Vitamin D therapy may be useful in the management of COPD, based on its ability to reduce inflammatory substances (cytokines) that play a major role in the pathology of this disease.
In the past few years, several studies have taken a look at the patterns of asthma diagnoses in various populations. An April 2009 study noted that Vitamin D is vital to proper lung development and that children with adequate levels of sun exposure and Vitamin D are less likely to suffer from wheezing illness. A scientific paper from 2007 turned its attention to the prevalence of asthma in modern times. A drastic increase in the number of asthmatics has been reported beginning in the 1960’s. Scientists theorize that this is likely due to more time spent indoors, perhaps because of growing concern about the risk of skin cancer. Attention is also spent on the finding that poor Vitamin D status in pregnant mothers can result in a 40% increased likelihood of asthma in their children. (2,3)
In May 2009, a study of 616 children in Costa Rica found a significant connection between insufficient amounts of Vitamin D and asthma. Higher levels of D were associated with a lower rate of allergies, less frequent hospitalization and “increased airway responsiveness. (4) The presence of allergies and asthma, as found in the Costa Rican study, is quite common. In research conducted in rats, Vitamin D supplementation has proven helpful against allergic asthma. (5) But more importantly, this trial is interesting because it analyzed children who live in a part of the world where sun deprivation is not considered a problem. Therefore, appropriate (Vitamin D) testing may be warranted even if regular sun exposure is present.

There are two other areas relating to pulmonary health that may be responsive to optimal levels of vitamin D. Here’s a brief review of both of them:
- Upper Respiratory Tract Infections: A February 2009 article in the Archives of Internal Medicine looked at the Vitamin D status of 883 varied individuals (12 years and older) over the course of 6 years. A clear pattern was found that indicates that people with the lowest amount of D contracted the greatest number of upper respiratory tract infections (URTIs). As the levels of Vitamin D increased, the occurrence of URTIs decreased. The authors noted that the association between D and URTIs was greater in those with preexisting lung conditions such as asthma and COPD. (6) However, it is important to note that a recent shorter term study using Vitamin D supplements did not significantly prevent URTIs. According to researchers, longer term studies are needed to help clarify the optimal dosage and most practical application of D. (7)
- Lung Cancer: Two epidemiological studies from 2008 found a pattern of infrequent UVB (sunlight ray) exposure and low levels of Vitamin D in the blood with a greater occurrence of lung cancer. One of the studies, based on analysis derived from 111 countries, verified this increased risk in both men and women. (8) A separate study that looked at Vitamin D blood levels only found a protective effect in women and younger individuals. (9) Once again, we’ll need more evidence to come to a firm conclusion about the role of Vitamin D in preventing lung cancer. Still, many researchers are quite optimistic about its potential. (10)
The sobering data on declining lung health should be enough to make us to take notice. In order to live an unrestricted and active life, we need a properly functioning pulmonary system. Every cell in the body absolutely requires the oxygen that our lungs provide. We may not be able to do a lot about the pollution in the air, but we can use the clues that science provides in order to protect every part of the body the best way we know how.
Note: Please check out the “Comments & Updates” section of this blog – at the bottom of the page. You can find the latest research about this topic there!
Be well!
JP
Tags: asthma, COPD, Vitamin D
Posted in Alternative Therapies, Heart Health, Nutritional Supplements

May 27th, 2009 at 11:06 am
We all tend to pay insufficient attention to vitamins, but their significance for the organism is actually huge! I have personally experienced what a great force, which have the potential of vitamins, in my case, vitamin D helped to cope with chronic illness.
May 27th, 2009 at 12:16 pm
Thanks for sharing your experience.
Be well!
JP
May 27th, 2009 at 2:18 pm
anyone interested in vitamin D should take a look at http://www.vitaminD3world.com It has some good summaries and offers a good newsletter.
May 27th, 2009 at 7:04 pm
Two excellent websites on vitamin d research:
http://www.vitamindcouncil.org
and
http://www.grassrootshealth.org
I have copd and vitamin d is the best thing that’s happened to me since I was diagnosed.
May 27th, 2009 at 9:42 pm
Thanks for your contribution, Mike.
Be well!
JP
May 27th, 2009 at 9:43 pm
Thank you, Deb!
I’m happy to know that Vitamin D is helping you maintain good health. Wonderful news!
Be well!
JP
May 27th, 2009 at 11:07 pm
Respiratory problems are my 90 yo mother’s weakness and she’s doing better since she’s upped her vitamin D and started sleeping on an antimicrobial Cupron pillowcase. One aggravating factor is that she’s on a proton pump inhibitor, which is known to promote pneumonia.
JP, here’s an article which discusses what is a safe vitamin D blood level. It appears that any level below 200 ng/ml is non-toxic.
http://ods.od.nih.gov/factsheets/vitamind.asp
May 27th, 2009 at 11:54 pm
I’m happy to hear about your mother’s success with D, Iggy.
Has your mom ever tried a PPI alternative? Maybe her symptoms could be managed by using a natural alternative.
Thanks for the link. It looks like a winner. 🙂
Be well!
JP
May 10th, 2011 at 12:10 pm
Has the result of the test mentioned here been published? Did I miss it somewhere?
May 15th, 2011 at 1:02 pm
Pat,
Can you please clarify what test you’re referring to?
Be well!
JP
October 26th, 2017 at 12:10 pm
Updated 10/26/17:
http://journals.lww.com/hnpjournal/Abstract/2017/11000/The_Effect_of_Progressive_Relaxation_Exercises_on.3.aspx
Holist Nurs Pract. 2017 Nov/Dec;31(6):369-377.
The Effect of Progressive Relaxation Exercises on Fatigue and Sleep Quality in Individuals With COPD.
This randomized controlled experimental study was conducted to investigate the effect of progressive muscle relaxation exercises on dyspnea, fatigue, and sleep quality in individuals with chronic obstructive pulmonary disease. A Descriptive Questionnaire and the Chronic Obstructive Pulmonary Disease and Asthma Fatigue Scale, Chronic Obstructive Pulmonary Disease and Asthma Sleep Scale and Medical Research Council Dyspnea Scale were used for data collection. The decrease in the mean dyspnea, fatigue, and sleep scores in the intervention group was statistically significantly more pronounced than the patients in the control group (P < .05). Progressive relaxation exercises can be implemented to decrease the dyspnea, fatigue, and sleep problems seen in patients with moderate and advanced chronic obstructive pulmonary disease by nurses working in the clinic. Be well! JP