Diabetes, GERD and Overeating Updates
June 11, 2010 Written by JP [Font too small?]It’s been over a year and half since I first started writing columns for HealthyFellow.com. Since this site’s inception, I’ve posted hundreds of blogs dealing with every conceivable facet of natural health and wellness. I believe that the majority of what I cover here has lasting power. I choose my sources of information carefully, which gives me confidence that the data I present will remain relevant for the foreseeable future. However, that doesn’t preclude me from updating new developments regularly for virtually every topic I’ve examined in the past. Medicine, be it alternative or conventional, stands still for no one.

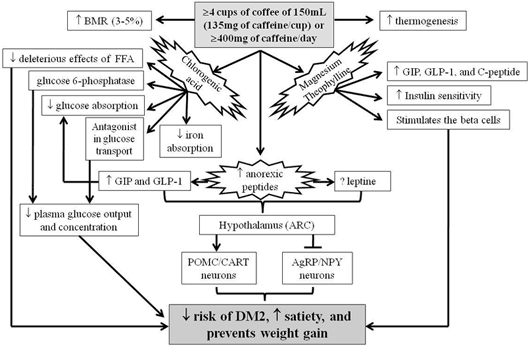
If there was a spell that could be cast that would eliminate diabetes from the face of the Earth, it would save hundreds of thousands of lives each year and spare a great deal of economic hardship and suffering for individuals and nations alike. The closest thing to magic in the field of diabetes management is adopting a healthy diet and lifestyle. And when comes to healthy beverages, coffee tops the list. The latest study to confirm this fact was conducted in an animal model. Japanese scientists gave diabetic mice a standard diet along with either regular drinking water or diluted coffee for 5 weeks. The mice fed the coffee blend demonstrated improved insulin sensitivity and lower blood sugar levels. There was also a reduction in inflammatory markers found in the fatty tissue of the coffee-fed mice. In addition, coffee appeared to reduce fat build up in the liver. Similar results have been reported in human populations as well. It’s important to note that caffeine is unlikely the only active ingredient in coffee that promotes diabetic health. A recent publication in the Journal of Agricultural Food Chemistry determined that chlorogenic acid, a phytochemical found in caffeinated and decaffeinated coffee, may inhibit the activity of an enzyme (glucose-6-phosphatase) which lowers the amount of sugar produced by the liver. The bottom line is that caffeine intolerance isn’t necessarily a reason to avoid drinking coffee altogether – especially if you’re at risk for diabetes. (1,2,3)
Last Friday I reported on the potential health risks associated with stomach acid suppressing medications or proton pump inhibitors. I presented a number of possible alternatives, but failed to mention the advantage of adopting a low carbohydrate diet. As early as 2001 there have been published case reports documenting the alleviation of gastroesophageal reflux (GERD) symptoms in patients following “self-initiated” low carb menu plans. In 2006 a formal trial confirmed the positive influence of restricting carbohydrates (20 grams or less/day) in a pilot study involving 8 patients living with GERD. Objective improvements were evidenced within 6 days, as measured by several tests including the GERD Symptom Assessment Scale. The concluding remarks of the authors state: “These data suggest that a very-low carbohydrate diet in obese individuals with GERD significantly reduces distal esophageal acid exposure and improves symptoms”. (4,5)
In November 2009 I wrote a column entitled, The Forgotten Superfruit about dried plums or prunes. Scientists from the Agricultural University of Athens, Greece recently looked into the validity of using a pre-meal snack of prunes as a way of reducing overall caloric intake. A total of 45 men and women took part in this randomized, crossover study. The trial required that the participants eat a pre-meal snack of prunes or a calorically equivalent bread snack on separate occasions. The findings of the experiment indicate that:
- Eating prunes resulted in lower caloric consumption during the following meal, especially with respect to dessert intake.
- Prune consumption also reduced subjective feelings of hunger and “motivation to eat“.
The researchers believe that the fiber content of prunes is likely responsible for the noted difference in dining patterns. That may be true, but there’s more to prunes than just dietary fiber. As I’ve noted in a previous column, prunes also provide a healthy concentration of antioxidants and nutrients. What’s more, they appear to be especially helpful for those prone to constipation and may even support skeletal health and, thereby, reduce the risk of fractures, osteopenia and osteoporosis. (6)
I love receiving email tips from my readers. It’s impossible for me to catch every relevant news item that’s out there. But with your assistance, I’ve got a much better shot. So please keep sending your valuable input and leads. You can always reach me directly at: jp@healthyfellow.com. I look forward to hearing from you!
Note: Please check out the “Comments & Updates” section of this blog – at the bottom of the page. You can find the latest research about this topic there!
Be well!
JP
Tags: Diabetes, GERD, Low Carb, Prunes
Posted in Bone and Joint Health, Diabetes, Diet and Weight Loss

June 11th, 2010 at 9:56 pm
You are as knowledgeable
as any nurse I know…
And lots nicer!
June 11th, 2010 at 10:32 pm
You’re too kind, Anne! 🙂
Thank you for all your kindness and support. It’s much appreciated!
Be well!
JP
June 12th, 2010 at 5:00 am
Good Morning, JP 🙂
sometimes i wish we would live next to you both, so we could meet us to cook low carb or just talk about all the news….would be funny and interesting…. 😉
About the prunes: i think or i hope the same is with apricots, at the moment our supermarket has lots of fresh organic apricots, they are so tasty ☼
wish you and yours a lovely weekend ☼☼☼
Nina K.
June 12th, 2010 at 12:27 pm
Good day, Nina!
It would indeed. 🙂
When I was growing up, my parents had a few fruit trees in their backyard. Apricot trees seemed to be some of the best producers. I have fond memories of eating them back then.
BTW, my dad and mom still have a thriving, little garden. They regularly eat homegrown salad and a variety of fruits and veggies.
I wish you and your husband the same! Enjoy!
Be well!
JP
June 12th, 2010 at 5:52 pm
I have an RSS feed to your blog and enjoy your views very much. I like the scientific basis you present.
Re: GERD. I have been on a health-improvement program since March of 2009 – exercising more and eating better. Thus far I have lost 81 pounds, and significantly reduced my acid reflux, with a lower carb plan where I totally cut out added sugars but still ate very limited grains.
About 45 days ago, I cut out all grains. I have been trying to get off my daily omprezole for some time, but every time I tried I would get severe reflux and would re-start. Shortly after cutting out the grains, I went off the daily omprezole and, after having to use TUMS a few times, haven’t needed anything for at least a month for acid reflux. This is amazing to me. I can hardly believe I am writing it.
Please keep up the good and significant work.
June 13th, 2010 at 5:22 am
JP, I always find you to be flexible in your views, looking at both sides of a nutritional issue. The information you’ve presented has been a great value to me in my quest to be more “natural” in nutrition and health. Keep up the good fight.
June 13th, 2010 at 12:58 pm
Thank you, Cassandra! I appreciate your kind words very much! 🙂
Your inspiring experience is reflected in the medical literature:
http://www.ncbi.nlm.nih.gov/pubmed/16279563
Some people may have undiagnosed food allergies and sensitivities that can cause GERD symptoms.
I’m happy to know that you’ve found your root cause and that you’ve addressed it with successful results. Excellent!
Be well!
JP
June 13th, 2010 at 1:02 pm
Thank you, Mark!
I really appreciate your participation on my site and all your support. 🙂
Be well!
JP
June 14th, 2010 at 7:58 am
Good Day JP!
A very useful article about the coffee and Diabetes connection! Most Type 2 Diabetics (Including myself) suffer from the sugar produced by the Liver. You would have a good exercise and your bedtime blood sugar reading would be 150 after meals, and around 2 am in the morning it would be around 100 (around 2 am is when the Circadian rythm kicks in and body’s biological clock starts ticking..and hormones etc would start their work), but the morning number would be 140-150 because of the “Dawn Syndrome” (Sugar dumped by the liver). I am certainly going to try the coffee. I currently do not drink coffee at all. JP any updates/research or tips about this “dawn Syndrome” would be very helpful! This is a start for sure and i will update..
Best Regards
Sai.
June 14th, 2010 at 12:13 pm
Thank you, Sai! 🙂
I’ll keep an eye out for new research on “dawn syndrome” and post what I find.
I hope your coffee experiment is successful!
Be well!
JP
June 14th, 2010 at 1:48 pm
Thanks much JP for adding that to your list!
Best Regards
Sai.
June 14th, 2010 at 3:42 pm
Any time, Sai! 🙂
This is an important issue with ramifications that affect a great many people.
Be well!
JP
January 3rd, 2012 at 8:35 pm
JP,
What a great article! Very informative and up to date. I consume a lot of coffee a day so I should be fine.
Love reading your articles and learning so many new theories and trials.
Thank you so much,
January 4th, 2012 at 2:29 pm
Thank you, Cynthia! 🙂
Be well!
JP
July 16th, 2015 at 9:18 pm
Updated 07/16/15:
http://www.ncbi.nlm.nih.gov/pubmed/26175057
Dis Esophagus. 2015 Jul 14.
Adherence to a predominantly Mediterranean diet decreases the risk of gastroesophageal reflux disease: a cross-sectional study in a South Eastern European population.
Our aim was to assess the association of a Mediterranean diet and gastroesophageal reflux disease among adult men and women in Albania, a former communist country in South Eastern Europe with a predominantly Muslim population. A cross-sectional study was conducted in 2012, which included a population-based sample of 817 individuals (≥18 years) residing in Tirana, the Albanian capital (333 men; overall mean age: 50.2 ± 18.7 years; overall response rate: 82%). Assessment of gastroesophageal reflux disease was based on Montreal definition. Participants were interviewed about their dietary patterns, which in the analysis was dichotomized into: predominantly Mediterranean (frequent consumption of composite/traditional dishes, fresh fruit and vegetables, olive oil, and fish) versus largely non-Mediterranean (frequent consumption of red meat, fried food, sweets, and junk/fast food). Logistic regression was used to assess the association of gastroesophageal reflux disease with the dietary patterns. Irrespective of demographic and socioeconomic characteristics and lifestyle factors including eating habits (meal regularity, eating rate, and meal-to-sleep interval), employment of a non-Mediterranean diet was positively related to gastroesophageal reflux disease risk (fully adjusted odds ratio = 2.3, 95% confidence interval = 1.2-4.5). Our findings point to a beneficial effect of a Mediterranean diet in the occurrence of gastroesophageal reflux disease in transitional Albania. Findings from this study should be confirmed and expanded further in prospective studies in Albania and in other Mediterranean countries.
Be well!
JP
August 15th, 2015 at 4:00 pm
Updated 08/15/15:
http://onlinelibrary.wiley.com/doi/10.1111/dote.12390/full
Dis Esophagus. 2015 Jul 30.
Short-term and long-term effect of diaphragm biofeedback training in gastroesophageal reflux disease: an open-label, pilot, randomized trial.
This study investigated the effectiveness of diaphragm biofeedback training (DBT) for patients with gastroesophageal reflux disease (GERD). A total of 40 patients with GERD treated at the Peking Union Medical College Hospital between September 2004 and July 2006 were randomized to receive DBT and rabeprazole proton pump inhibitor (PPI) or rabeprazole alone. The DBT + rabeprazole group received DBT during the 8-week initial treatment; the rabeprazole group did not. During the 6-month follow up, all patients took acid suppression according to their reflux symptoms, and the patients in the DBT + rabeprazole group were required to continue DBT. The primary outcome (used for power analysis) was the amount of acid suppression used at 6 months. Secondary outcomes were reflux symptoms, health-related quality of life (HRQL), and esophageal motility differences after the 8-week treatment compared with baseline. Acid suppression usage significantly decreased in the DBT + rabeprazole group compared with the rabeprazole group at 6 months (P < 0.05). At 8 weeks, reflux symptoms and GERD-HRQL were significantly improved in both groups (P < 0.05), without difference between them. Crural diaphragm tension (CDT) and gastroesophageal junction pressure (GEJP) significantly increased in the DBT + rabeprazole group (P < 0.05), but without change in lower esophageal sphincter (LES) pressure. There was no significant change in CDT, GEJP, and LES pressure compared with baseline in the rabeprazole group. In conclusion, long-term DBT could reduce acid suppression usage by enhancing the anti-reflux barrier, providing a non-pharmacological maintenance therapy and reducing medical costs for patients with GERD. Be well! JP
June 26th, 2016 at 8:23 pm
Updated 06/26/16:
http://www.mdpi.com/2072-6643/8/6/350/htm
Nutrients. 2016 Jun 8;8(6). pii: E350.
Flavonoids, Flavonoid Subclasses, and Esophageal Cancer Risk: A Meta-Analysis of Epidemiologic Studies.
Flavonoids have been suggested to play a chemopreventive role in carcinogenesis. However, the epidemiologic studies assessing dietary intake of flavonoids and esophageal cancer risk have yielded inconsistent results. This study was designed to examine the association between flavonoids, each flavonoid subclass, and the risk of esophageal cancer with a meta-analysis approach. We searched for all relevant studies with a prospective cohort or case-control study design published from January 1990 to April 2016, using PUBMED, EMBASE, and Web of Science. Pooled odds ratios (ORs) were calculated using fixed or random-effect models. In total, seven articles including 2629 cases and 481,193 non-cases were selected for the meta-analysis. Comparing the highest-intake patients with the lowest-intake patients for total flavonoids and for each flavonoid subclass, we found that anthocyanidins (OR = 0.60, 95% CI: 0.49-0.74), flavanones (OR = 0.65, 95% CI: 0.49-0.86), and flavones (OR = 0.78, 95% CI 0.64-0.95) were inversely associated with the risk of esophageal cancer. However, total flavonoids showed marginal association with esophageal cancer risk (OR = 0.78, 95% CI: 0.59-1.04). In conclusion, our study suggested that dietary intake of total flavonoids, anthocyanidins, flavanones, and flavones might reduce the risk of esophageal cancer.
Be well!
JP
June 27th, 2016 at 9:46 pm
Updated 06/27/16:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4908257/
J Diabetes Res. 2016;2016:5147468.
Silymarin in Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis of Randomized Controlled Trials.
Type 2 diabetes mellitus (T2DM) is associated with increased risk of cardiovascular disease and nephropathy-now the leading cause of end-stage renal disease and dialysis in Europe and the United States. Inflammation and oxidative stress play a pivotal role in the development of diabetic complications. Silymarin, an herbal drug with antioxidant and anti-inflammatory properties, may improve glycemic control and prevent the progression of the complications. In a systematic review and meta-analysis including five randomized controlled trials and 270 patients, routine silymarin administration determines a significant reduction in fasting blood glucose levels (-26.86 mg/dL; 95% CI -35.42-18.30) and HbA1c levels (-1.07; 95% CI -1.73-0.40) and has no effect on lipid profile. Benefits for silymarin on proteinuria and CKD progressions are reported in only one small study and are uncertain. However, being aware of the low quality of the available evidence and elevated heterogeneity of these studies, no recommendation can be made and further studies are needed.
Be well!
JP
April 11th, 2017 at 6:05 pm
Updated 04/11/17:
http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0174820
PLoS One. 2017 Apr 3;12(4):e0174820.
The effect of meal frequency in a reduced-energy regimen on the gastrointestinal and appetite hormones in patients with type 2 diabetes: A randomised crossover study.
BACKGROUND: Appetite and gastrointestinal hormones (GIHs) participate in energy homeostasis, feeding behavior and regulation of body weight. We demonstrated previously the superior effect of a hypocaloric diet regimen with lower meal frequency (B2) on body weight, hepatic fat content, insulin sensitivity and feelings of hunger compared to the same diet divided into six smaller meals a day (A6). Studies with isoenergetic diet regimens indicate that lower meal frequency should also have an effect on fasting and postprandial responses of GIHs. The aim of this secondary analysis was to explore the effect of two hypocaloric diet regimens on fasting levels of appetite and GIHs and on their postprandial responses after a standard meal. It was hypothesized that lower meal frequency in a reduced-energy regimen leading to greater body weight reduction and reduced hunger would be associated with decreased plasma concentrations of GIHs: gastric inhibitory peptide (GIP), glucagon-like peptide-1(GLP-1), peptide YY(PYY), pancreatic polypeptide (PP) and leptin and increased plasma concentration of ghrelin. The postprandial response of satiety hormones (GLP-1, PYY and PP) and postprandial suppression of ghrelin will be improved.
METHODS: In a randomized crossover study, 54 patients suffering from type 2 diabetes (T2D) underwent both regimens. The concentrations of GLP-1, GIP, PP, PYY, amylin, leptin and ghrelin were determined using multiplex immunoanalyses.
RESULTS: Fasting leptin and GIP decreased in response to both regimens with no difference between the treatments (p = 0.37 and p = 0.83, respectively). Fasting ghrelin decreased in A6 and increased in B2 (with difference between regimens p = 0.023). Fasting PP increased in B2with no significant difference between regimens (p = 0.17). Neither GLP-1 nor PYY did change in either regimen. The decrease in body weight correlated negatively with changes in fasting ghrelin (r = -0.4, p<0.043) and the postprandial reduction of ghrelin correlated positively with its fasting level (r = 0.9, p<0.001). The postprandial responses of GIHs and appetite hormones were similar after both diet regimens.
CONCLUSIONS: Both hypocaloric diet regimens reduced fasting leptin and GIP and postprandial response of GIP comparably. The postprandial responses of GIHs and appetite hormones were similar after both diet regimens. Eating only breakfast and lunch increased fasting plasma ghrelin more than the same caloric restriction split into six meals. The changes in fasting ghrelin correlated negatively with the decrease in body weight. These results suggest that for type 2 diabetic patients on a hypocaloric diet, eating larger breakfast and lunch may be more efficient than six smaller meals during the day.
Be well!
JP
August 25th, 2017 at 2:10 pm
Updated 08/25/17:
https://www.ncbi.nlm.nih.gov/pubmed/28835761
Int J Endocrinol Metab. 2017 Jan 21;15(1):e40614.
The Effect of n-3 Polyunsaturated Fatty Acids Supplementation on Serum Irisin in Patients with Type 2 Diabetes: A Randomized, Double-Blind, Placebo-Controlled Trial.
BACKGROUND: Diabetes refers to a group of metabolic diseases with blood glucose of higher than normal ranges. Furthermore, n-3 polyunsaturated fatty acids are necessary for the regulation of the activity of human function. The effect of n-3 PUFA on diabetes has been investigated in animal studies, yet, the exact amount has not been set, to date. Irisin, as a new myokine, is released from skeletal muscle and Irisin levels decrease as a result of physical inactivity, overweightness, and obesity. Also, the reduction of serum irisin level is associated with development of insulin resistance and type 2 diabetes. This study was performed to assess the effects of n-3 PUFA supplementation on serum irisin level in patients with diabetes.
METHODS: This randomized clinical trial included 43 patients with type 2 diabetes (21 patients in the placebo group and 22 patients in the n-3 PUFA supplement group). They were randomized to groups, one receiving 10 weeks of either n-3 PUFA supplement and the other the placebo (1250 mg capsule, three times per day). Samples were also matched by age, gender, and body mass index (BMI) in the 2 groups. Anthropometric measurements, demographic information and dietary intakes were obtained both before and after the intervention. Serum irisin levels were measured before and after the intervention using human irisin enzyme linked immunosorbent assay (ELISA) kit. Independent t-test was used to compare the mean outcomes between groups.
RESULTS: At baseline, irisin serum levels were not significantly different between the placebo and n-3 PUFA supplementation groups (P > 0.05). However, a significant change was observed between the groups after intervention (P = 0.04). Also there was a significant difference in mean change (after versus before the intervention) (P = 0.05). Compared to the placebo, n-3 PUFA supplementation decreased serum FBS and HbA1C (P = 0.036 and 0.001; respectively). Also, there were significant differences between changes of diastolic blood pressure and HOMA-IR after the intervention between the groups. The duration of illness was not considered as a confounding factor because there was no significant association between irisin level (after versus before the intervention) and the illness duration.
CONCLUSIONS: The current study indicated that n-3 PUFA supplementation with a dosage of 1250 mg three times per day, resulted in increased serum irisin level of diabetic patients.
Be well!
JP